How Does Chiropractic Adjustment Work? What to Expect
You wake up already stiff. Maybe your lower back grabs when you lean over the sink. Maybe your neck still feels wrong weeks after a car accident. Maybe you're walking the Deerfield Beach boardwalk more carefully than you used to because your hips, knees, or spine don't feel as steady.
That kind of pain is frustrating because it doesn’t just hurt. It changes how you move, sleep, work, drive, and even how long you can stand in the kitchen.
A lot of people in that spot start asking the same question: how does chiropractic adjustment work, really? Is it just “cracking” joints? Is the popping sound the whole treatment? Why do some people feel looser right away while others feel sore first?
Those are fair questions. Chiropractic care has been around since 1895, when Daniel David Palmer performed the first adjustment, and today millions of people still use it because they want a non-surgical, hands-on way to reduce pain and move better. If your discomfort also gets worse at night, sleep setup matters too. Many patients find it helpful to review practical guidance on an orthopaedic mattress for pain relief, because what supports your spine for eight hours can affect how you feel the next morning.
The important part is this: an adjustment isn’t random force. It’s a specific movement applied to a joint that isn’t moving the way it should. The goal is to improve motion, calm irritated tissues, reduce protective muscle guarding, and help your nervous system stop treating normal movement like a threat.
Once you understand that, chiropractic care starts to make a lot more sense. It becomes less about noise and more about mechanics, muscle tone, nerve signaling, and what your body needs to move comfortably again.
The Hidden Story Behind Your Aches and Pains
Aches often begin subtly. A long commute. A weekend project. One awkward lift. A fender bender that seemed minor at the time. Then your body adapts in ways you may not notice at first.
You bend less through one part of your spine and more through another. Your shoulder tightens to protect your neck. Your low back muscles stay “on” all day because one joint isn’t gliding well. Soon, something simple like getting out of bed or turning to check traffic starts to feel harder than it should.
Pain isn’t always just about injury
Pain is often assumed to mean something is torn, broken, or badly damaged. Sometimes that’s true. Often, though, the problem is more functional than dramatic.
A joint can become restricted, meaning it still moves, just not normally. Think of a door hinge that opens, but sticks halfway and squeaks every time you use it. The door isn’t broken. It just isn’t moving cleanly.
That matters because joints, muscles, and nerves work as a team. When a spinal joint loses smooth motion, nearby muscles often tighten to guard it. The irritated area becomes more sensitive. Your brain starts paying more attention to that region, and ordinary movement begins to feel threatening.
Many people don’t seek care because the pain is unbearable. They seek care because they’re tired of planning their day around it.
Why symptoms spread beyond one spot
Confusion often arises. People feel pain in the hip, buttock, shoulder blade, or leg and assume the problem must live exactly there. Sometimes it does. Sometimes the underlying cause is a restricted spinal or pelvic joint changing how everything around it moves.
Common examples include:
- Low back pain that travels into the buttock or thigh because irritated tissues and tight muscles change movement patterns.
- Neck stiffness after an accident that leads to headaches, shoulder tension, or trouble turning the head while driving.
- Arthritic stiffness that isn’t constant all day, but flares when joints sit too long and then have to start moving again.
Pain also has a way of creating fear. People stop walking as far. They stop exercising. They brace when they bend. That protective behavior makes sense, but over time it can make the body even stiffer and weaker.
A chiropractic adjustment aims to interrupt that cycle. Not by “putting bones back in place” in a simplistic sense, but by restoring better motion, reducing unnecessary muscle guarding, and helping the nervous system accept movement again.
Understanding the Chiropractic Adjustment at Its Core
You lie on the table, the chiropractor checks the area that feels stuck, and then comes a quick, precise movement. Sometimes there is a pop. Sometimes there is not. What matters is that the input is specific, controlled, and aimed at helping a restricted joint move more normally again.
A chiropractic adjustment is a precise therapeutic movement applied to a joint that is not gliding or rotating the way it should. The point is not noise. The point is to give your body a clean mechanical signal that can change motion, muscle tension, and the way your nervous system reads that area.
A helpful comparison is a door hinge that has started sticking. The problem is rarely that the whole door is in the wrong house. The hinge is not moving well, so the frame, handle, and the person pushing the door all have to work harder. A restricted spinal or extremity joint creates a similar chain reaction.
What chiropractors are actually treating
The treatment target is usually a joint restriction. That means a spinal or extremity joint has lost some of its normal quality of motion. It may still move a little, but not smoothly, not comfortably, and not in good coordination with nearby tissues.
That loss of motion can contribute to:
- Pain, because irritated joints and surrounding tissues send more danger signals
- Muscle tightness, because the body braces around an area it does not trust
- Stiffness, especially after sitting, sleeping, or repetitive activity
- Compensation, where nearby joints and muscles do extra work
If you’re new to the profession, this overview of what a chiropractor does can help separate common myths from the actual clinical role.
The adjustment is specific in contact, direction, and timing
People often hear the word “adjustment” and picture a big twist. In practice, the movement is much smaller and more exact than that. The doctor sets up the contact point, preloads the joint gently, and delivers a brief thrust within the joint’s normal anatomical limits.
A common method is a high-velocity, low-amplitude thrust, often shortened to HVLA. “High velocity” refers to speed. “Low amplitude” means the movement itself is very short. That combination matters because the body often responds better to a quick, well-placed input than to a long shove.
Precision changes the experience. It also changes the effect.
Why that quick input can change so much
A restricted joint affects more than bone position. It affects the sensors in and around the joint, the tone of nearby muscles, and the messages traveling to the central nervous system.
Here is a simplified version of what can happen:
- A joint stops moving well
- Nearby muscles tighten to protect it
- Motion feels less predictable, so the area becomes more sensitive
- A precise adjustment delivers a fast mechanical signal
- Joint receptors and muscle reflexes respond
- The brain gets updated information that the area can move with less threat
This is one reason adjustments can feel surprisingly different from stretching. Stretching usually asks a guarded area to lengthen. An adjustment gives the nervous system a brief, targeted event that can reset how that area is being managed.
One piece of that response may involve the Golgi tendon organs, or GTOs, which are sensory receptors in tendons that help regulate muscle tension. When the surrounding tissues experience a rapid, specific change, those receptors can contribute to a reduction in protective muscle guarding. The result is often a feeling of easier motion, not because a muscle was forced to relax, but because the body no longer feels the same need to hold on so tightly.
The pop is optional. The response is the point.
People often focus on whether they heard a sound. The sound can happen, but it is not the measure of success. Many effective adjustments are quiet. Many patients also improve with instrument-assisted methods or mobilization techniques that do not create a pop at all.
What matters more clinically is whether the joint moves better afterward and whether the surrounding tissues calm down. That is why two patients with similar symptoms may receive different types of care. One person may need a hands-on spinal adjustment. Another may respond better to an instrument-assisted technique. A third may need soft tissue work first so the joint can accept the change.
What patients usually notice afterward
The first changes are often practical. Turning the head may feel easier. Standing up may feel less “caught.” Walking may feel more even.
Some patients also notice mild soreness later, similar to what you might feel after using a stiff area more normally for the first time in a while. That does not automatically mean something went wrong. It often reflects a body region adapting to a new movement pattern. At MedAmerica, that matters because the adjustment is rarely treated as a one-off event. It is used as part of a broader plan that may also include rehab exercise, soft tissue care, and guidance on what to do after the visit so the improvement lasts.
The goal is simple. Help the joint move better, help the nervous system trust that movement again, and make daily activity feel easier and safer.
The Science of How Adjustments Relieve Pain
A patient comes in because turning to check a blind spot hurts, and by the end of the visit that same movement feels easier and less guarded. That change can seem sudden, but it is not random. An adjustment affects joint motion, muscle tension, and the way the nervous system processes threat signals from that area.
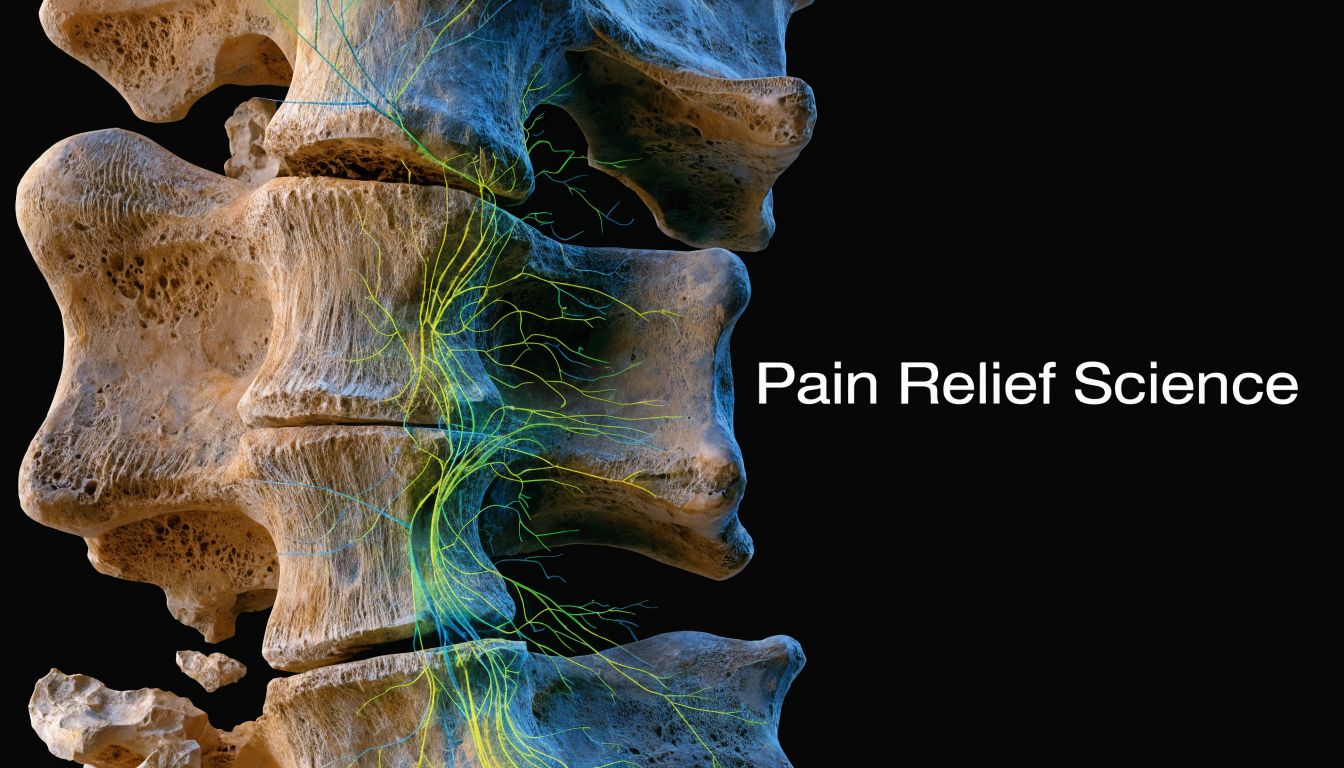
The mechanical effect of a restricted joint moving again
Start with the joint itself.
When a spinal segment is not moving well, nearby tissues often compensate. Muscles tighten, movement becomes uneven, and simple motions like bending, reaching, or turning can start to feel blocked. An adjustment gives that restricted segment a quick, specific input that can restore a more normal glide between the joint surfaces.
Sometimes there is a pop. That sound is called cavitation, which happens when pressure changes inside the joint fluid. The sound is only a side effect. The part that matters is better motion.
A stuck jar lid works as a good comparison. The click is not the goal. The goal is that the lid turns again. In the same way, the useful change after an adjustment is that the joint stops resisting normal movement so strongly.
The muscle response and the role of Golgi Tendon Organs
The next layer involves muscle tone.
Muscles and tendons contain sensors that report tension and position to the spinal cord and brain. One of those sensors is the Golgi Tendon Organ, or GTO. It works like a tension monitor attached to the muscle-tendon unit.
A quick, well-placed adjustment can stimulate these sensors and change the reflex activity around the joint. That input may reduce overactive muscle guarding through a mechanism often described as autogenic inhibition, as explained in Adjust My Pain’s discussion of GTO activation during chiropractic adjustment. In plain language, a muscle that has been gripping for protection may finally get the message that it can ease off.
Patients often describe this as, “It feels like it let go.”
That feeling matters because painful stiffness is often a mix of true joint restriction and protective muscle bracing. If the joint moves a bit better but the muscle still acts like a bodyguard, relief will be limited. If both change together, movement usually feels lighter and less threatening.
Silent adjustments can still work very well. The therapeutic effect comes from the body’s response, not from the volume of the sound.
How the nervous system can turn the volume down on pain
Pain is not created by joints alone. The nervous system decides how much protection to apply.
Each joint has receptors that send position and movement information upward. If that input has been poor for a while, the brain may treat the area as unreliable and respond with more pain, more guarding, or both. A precise adjustment provides a strong burst of fresh sensory input, and that can influence how the central nervous system interprets the area.
That process is one reason researchers and clinicians talk about CNS modulation after an adjustment. Sensory signals from the adjusted joint can affect spinal cord processing, help interrupt a pain-amplifying pattern, and improve how the brain maps movement from that region, as outlined in The American Chiropractor’s explanation of CNS modulation after adjustment.
A practical way to picture this is a car alarm that has become too sensitive. It keeps sounding even when the threat is minor. Better sensory input can help recalibrate the system so it reacts more appropriately. In the body, that can mean less sharpness, less guarding, and smoother coordination.
For a visual look at spinal mechanics and why nerve-related pain can spread, this short video helps make the concept less abstract.
Why some people feel relief quickly, and what to expect after
Relief can happen quickly because several systems may change in the same visit.
| Effect | What changed | What you may notice |
|---|---|---|
| Mechanical | Joint motion improved | Less stiffness, easier turning or bending |
| Muscular | Guarding reduced | A released or lighter feeling |
| Neurological | Pain processing shifted | Less sharpness, better body awareness |
That early improvement is only part of the story. Some patients leave feeling freer right away. Others notice the bigger change later that day or the next morning, once the area has had time to settle. Mild soreness can happen, especially if the region has been moving poorly for a long time. That response usually feels more like post-exercise soreness than injury pain.
At MedAmerica, that “what happens after” piece matters. We do not treat the adjustment as an isolated event. We often pair it with exercise, soft tissue treatment, and movement retraining so the nervous system keeps getting the message that the area is safe to use. If a patient needs a gentler approach, options such as instrument-assisted chiropractic care with the ArthroStim can deliver a precise input without the feel of a traditional manual thrust.
That is why a good adjustment is more than a quick pop. It is a targeted neurophysiological reset, followed by the right support so pain relief and improved mobility have a better chance to last.
Exploring Different Chiropractic Adjustment Techniques
Not every adjustment looks or feels the same. Chiropractors use different techniques because people present with different ages, conditions, comfort levels, and movement patterns.
One patient wants a traditional hands-on adjustment. Another is nervous about twisting. A third has significant stiffness and does better with a more measured approach. Good care adapts the tool to the patient.
The main styles patients are likely to hear about
Some techniques rely on a manual thrust from the chiropractor’s hands. Others use a handheld instrument that delivers a quick impulse. Neither method is automatically better. The best option depends on the body in front of the clinician.
A few common examples include:
Diversified technique
This is the classic hands-on chiropractic adjustment many people picture. It uses a quick, specific thrust to improve motion in a restricted joint. Patients often notice an immediate sense of release.Gonstead technique
This approach is known for careful analysis and precise setup. The movement is still specific, but the emphasis is on exact contact and line of correction.Activator or instrument-assisted methods
These use a spring-loaded or electronically assisted device to deliver a small, fast impulse. They’re often a good fit for seniors, people who prefer a gentler feel, or patients who are sensitive after injury.
If you’re curious about instrument-based care, this overview of the benefits of using the ArthroStim instrument for chiropractic therapy gives a practical look at why some clinics choose it.
Common Chiropractic Adjustment Techniques
| Technique | Method | Best For | What It Feels Like |
|---|---|---|---|
| Diversified | Manual HVLA thrust to a specific joint | General spinal stiffness, back pain, neck pain | Quick movement, sometimes with a pop |
| Gonstead | Precise manual correction based on focused analysis | Patients who benefit from highly specific segmental correction | Controlled and targeted, often very exact |
| Activator | Handheld instrument delivers a rapid impulse | Seniors, sensitive patients, those wary of manual thrusts | Light tapping or clicking sensation |
| ArthroStim style instrument-assisted care | Repetitive gentle impulses through a device | Guarded muscles, tender areas, patients needing lower-force input | Fast gentle pulses rather than one larger thrust |
Why chiropractors don’t use one method for everyone
Technique choice often comes down to three practical questions.
First, how irritated is the area? A person with fresh whiplash may need a very different approach than someone with long-term mid-back stiffness.
Second, how much force is appropriate? Some bodies respond beautifully to manual adjustments. Others relax better when force is lighter and more repetitive.
Third, what does the patient tolerate well? The best adjustment is one that is safe, specific, and appropriate. It doesn’t need to look dramatic to work.
A gentle technique isn’t a lesser technique. Sometimes it’s the smartest one.
Technique is only the delivery system. The underlying purpose remains the same: improve joint motion, reduce guarding, and help the body move with less pain.
Who Benefits Most From Chiropractic Care
Chiropractic care tends to help people whose pain is tied to joint restriction, mechanical stress, muscle guarding, and irritated movement patterns. That includes many adults with back and neck pain, but it also reaches further than that.

A major example is low back pain. A 2018 JAMA Network Open study found that patients receiving chiropractic adjustments were more likely to report a substantial reduction in pain intensity of more than 30% compared with usual medical care, and related data also notes that 90% of patients report significant low back pain relief after six weeks of treatment, according to the American Chiropractic Association research summary.
Common situations where adjustments may help
People often benefit when they have symptoms like these:
- Chronic low back pain that flares with sitting, lifting, or getting up from bed
- Sciatica-type symptoms where pain, tingling, or tightness travels from the low back into the leg
- Neck pain and whiplash after an auto accident, especially when turning the head feels restricted
- Tension headaches related to neck and upper back stiffness
- Arthritic stiffness where motion is limited and the body feels better once it gets moving
- Sports-related joint restriction that affects mechanics during training
- Age-related mobility decline when spinal or extremity stiffness contributes to balance problems
Why the right patient often notices the biggest change
The people who tend to respond best are those whose symptoms are strongly linked to movement.
For example, if your pain is worst when you first stand up, when you turn in the car, when you roll in bed, or when you try to bend and straighten again, there’s often a mechanical component. Chiropractic care aims at that mechanical component directly.
This doesn’t mean every painful condition should be adjusted. Good clinical judgment matters.
When an adjustment may not be appropriate
There are times when a chiropractor may modify care, delay treatment, or refer out first. That can include suspected fracture, severe instability, certain serious medical conditions, or symptoms that suggest the pain is not primarily mechanical.
That caution is a strength, not a weakness. The right provider isn’t trying to force every problem into one treatment style. They’re deciding whether a chiropractic adjustment fits the situation safely and sensibly.
The best candidate for chiropractic care isn’t “anyone with pain.” It’s the person whose pain pattern matches a problem with motion, mechanics, and muscle guarding.
It’s not only for one age group
Adults in desk jobs, retirees trying to stay active, people recovering from accidents, and recreational athletes can all be good candidates. The technique and treatment plan may look different, but the clinical reasoning is similar. Improve motion, reduce irritation, and help the body handle daily activity with less strain.
Your First Appointment and Post-Adjustment Care
For many new patients, the biggest fear isn’t the treatment itself. It’s not knowing what’s going to happen.
A first visit usually starts with questions. Where does it hurt? When did it begin? What movements make it worse? Have you had a fall, an accident, surgery, numbness, or weakness? That conversation matters because the adjustment should match your history, symptoms, and exam findings.
If you want a fuller overview of the typical timeline, this guide to the process of chiropractic care is a useful primer before your visit.
What usually happens during the visit
Most first appointments include a combination of:
History and symptom review
The provider looks for patterns that suggest a mechanical problem, a nerve-related issue, or a reason to be cautious.Physical examination
This may include posture, joint motion, orthopedic tests, strength, reflexes, and palpation of tender or restricted areas.Explanation before treatment
You should know what the chiropractor plans to do and why. If a certain technique doesn’t feel right to you, say so.The adjustment itself
Depending on the technique, you may lie face down, on your side, seated, or supported by a specialized table. The movement is quick and specific.
What the adjustment feels like
Some people feel a pop. Some feel only pressure or a fast impulse. Some feel immediate looseness. Others notice the biggest difference later that day, when standing up or walking feels easier.
Afterward, your chiropractor may recommend a short walk, some light range-of-motion work, ice, hydration, or follow-up therapy. Thoughtful clinics also pay attention to comfort and communication, and this article on how to enhance the patient experience in a chiropractic office highlights simple details that can make first visits feel much less intimidating.
What if you feel sore after
Mild soreness after a first adjustment is common. Verified data notes that up to 50% of new patients may feel soreness similar to starting a new exercise routine, and it typically lasts 24 to 48 hours, based on Cornerstone Family Chiropractic’s explanation of post-adjustment soreness.
That soreness usually doesn’t mean something went wrong. It often means tissues that were stiff or guarded are adapting to a new movement pattern.
A few simple responses usually help:
- Drink water if you tend to tense up and feel achy after treatment
- Take a light walk instead of lying still for the rest of the day
- Use ice on a sore area if it feels irritated
- Avoid testing it constantly by twisting or bending over and over to see if it’s “fixed”
Soreness after an adjustment should feel more like post-workout fatigue than sharp injury pain.
If pain feels severe, unusual, or concerning, contact the clinic and ask. New patients deserve clear expectations, not guesswork.
How Adjustments Integrate with Your Rehab Plan at MedAmerica
A good adjustment often creates an opening. The joint moves with less resistance, the surrounding muscles stop bracing as hard, and the nervous system gets a cleaner signal about where that area is in space. That change can reduce pain and improve mobility, but it also sets up the next part of treatment.
At MedAmerica, the goal is not to chase a pop. The goal is to use the adjustment at the right moment so exercise, soft tissue treatment, and other rehab tools work better afterward.

Why combined care often makes more sense
A stiff spinal segment can act like a rusted door hinge. You can force the door open, but it will still catch if the frame is crooked and the screws are loose. In the body, the joint is only one piece. The muscles around it may be tight, the stabilizers may be underperforming, and the brain may still expect pain with certain movements.
That is why a rehab plan often layers care instead of relying on one treatment alone. An adjustment may help reset motion and reduce protective muscle guarding through mechanisms like Golgi tendon organ input and central nervous system modulation. Once that happens, the body is often more ready to learn a better movement pattern.
Common pairings include:
- Physical therapy exercises to build control and strength after motion improves
- Soft tissue work to calm muscles that have stayed tense around the problem area
- Shockwave therapy for stubborn tendon or soft tissue irritation
- Balance and gait training for patients who need steadier movement, not just more movement
As noted earlier, chiropractic care is often associated with good value in musculoskeletal treatment. In practice, the biggest benefit of combining therapies is simple. Each treatment addresses a different part of the problem.
How the pieces support each other
Here is how that can look in real life.
If your low back has been locked up for weeks, an adjustment may restore enough motion that you can finally hinge, walk, or turn with less guarding. Right after that, guided rehab exercises teach your body how to keep using that new range. Without that follow-up, the area may drift back into the same protected pattern.
The same idea applies to neck pain, sciatica, post-accident injuries, and sports injuries. A manual adjustment can change the input coming from a painful joint. Exercise then helps your muscles and brain trust that movement again. Soft tissue care can reduce the pull from overworked muscles that would otherwise drag the area back into stiffness.
That sequence matters.
Patients often feel the difference as, "I can move more freely, and now the exercises make sense." That is a strong sign the treatments are supporting each other instead of competing with each other.
At MedAmerica, that coordinated approach is the point. If a clinician sees that a joint restriction is limiting your squat, gait, shoulder motion, or rehab tolerance, the adjustment is used to clear that roadblock. Then the next step in your plan reinforces the gain, whether that means corrective exercise, physical therapy, acupuncture, or another rehab service.
A good plan does more than reduce pain for a day. It helps your body keep the improvement.
If back pain, neck stiffness, sciatica, headaches, arthritis, or post-accident discomfort is limiting your daily life, MedAmerica Rehab Center offers a multidisciplinary approach that combines chiropractic care with physical therapy, acupuncture, and advanced rehab options. Their team has served Deerfield Beach since 1995, with personalized plans designed to relieve pain, restore mobility, and help you get back to normal activity with clear guidance from your first visit onward.

