What Is Dry Needling in Physical Therapy? A Patient Guide
Your back still tightens up by midday. Your neck feels stuck after hours at a desk. That sciatic pain runs down your leg even though you’ve tried rest, ice, stretching, and maybe a few YouTube exercises. A lot of people end up here. They’re doing their best, but the pain keeps coming back.
That’s often when someone asks, what is dry needling in physical therapy, and could it help me?
Dry needling is a modern treatment used by specially trained physical therapists to target painful muscle knots and movement problems. It isn’t a “last resort” or an alternative fringe idea. It’s a hands-on, anatomy-based technique used in mainstream rehab to help calm pain, improve motion, and make exercise more productive.
The key point is this. Dry needling is usually not the whole plan. It’s one tool inside a bigger recovery strategy that may also include movement retraining, strengthening, manual therapy, and education. When used that way, it can help patients with back pain, neck pain, sciatica, sports injuries, and other stubborn muscle-driven problems move forward faster.
Tired of Nagging Pain? A Different Approach to Relief
Many painful problems don’t come from a single dramatic injury. They build over time. A muscle stays guarded after an old strain. A shoulder never fully relaxes after repetitive overhead work. The low back starts compensating for weak hips, and now the same area keeps “locking up.”
In those cases, rest alone often doesn’t solve the underlying issue. Ice may calm things for a while. Stretching may feel good for an hour. Heat may loosen you up temporarily. Some people also explore options like sauna for pain relief because warmth can help sore tissues feel less stiff. But if a trigger point keeps reactivating, the body may need something more direct.
Why more patients are hearing about dry needling
Dry needling has become much more common in physical therapy. Approximately 50% of the 259,000 practicing physical therapists in the United States currently perform dry needling, and regulatory approval has grown to 38 states plus Washington, D.C. by 2024, reflecting wider acceptance in clinical practice and regulation, according to this dry needling adoption overview.
That matters to patients because it tells you this isn’t an obscure treatment. It’s a technique many licensed PTs have added to care for pain and movement problems that don’t respond well to simpler approaches.
Dry needling is best understood as a targeted physical therapy tool. It helps open a window for better movement, better exercise, and less pain.
When people usually ask about it
Patients often become curious about dry needling when they notice patterns like these:
- Recurring muscle knots: The same spot in the shoulder blade, calf, or upper trap keeps tightening.
- Pain with normal movement: Turning your head, bending forward, or reaching overhead feels restricted.
- Stalled progress in rehab: You’re doing exercises, but pain still blocks strength or mobility gains.
- Radiating discomfort: A tight muscle may also refer pain somewhere else, such as from the glutes into the leg.
That last point surprises many people. A “knot” in one area can create symptoms in another, which is one reason persistent pain can feel confusing.
How Dry Needling Works on Muscle Knots and Pain
A myofascial trigger point is a tight, irritable spot in a muscle. Patients usually call it a knot. That’s a useful way to think about it, as long as you picture something more active than a simple lump. It behaves more like a tiny section of muscle that won’t fully let go.
A trigger point can stay shortened, sensitive, and protective. That changes how the muscle pulls, how nearby joints move, and how your nervous system interprets pain. One irritated area can create stiffness, weakness, referred pain, or a deep ache that doesn’t match what the MRI or X-ray might show.
What the needle is actually doing
Dry needling uses thin filiform needles, typically 0.25 to 0.30 mm in diameter, to target those dysfunctional spots. The therapist places the needle into the trigger point to stimulate a local twitch response, which is an involuntary spinal reflex. A review described how this response can disrupt contracted muscle fibers, stimulate mechanoreceptors, improve local blood flow, and reduce pain sensitization through neurophysiological effects. The same review found dry needling was superior to sham or no treatment for short-term pain reduction in musculoskeletal conditions, as detailed in this open-access review of dry needling mechanisms and outcomes.
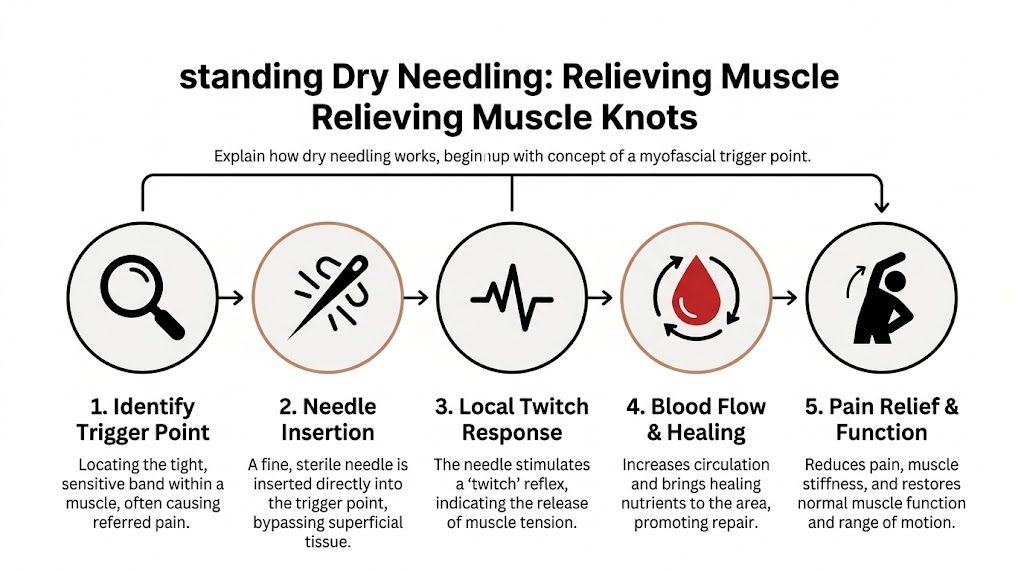
Dry needling reboots a glitchy muscle. The muscle has gotten stuck in an unhealthy pattern. The needle gives the nervous system a precise signal that helps interrupt that pattern.
The goal isn’t just to “poke the knot.” The goal is to help the muscle and nervous system stop overreacting so normal movement can return.
Why the twitch matters
Not every treatment creates a dramatic twitch, and that’s okay. But when it happens, patients often describe it as a quick cramp, jump, or deep ache. Clinically, that response suggests the therapist has engaged the sensitive tissue.
Afterward, many people notice that the area feels looser, lighter, or less guarded. Range of motion may improve right away. Pressure on the spot may feel less intense. If chronic tightness has been limiting your progress, this can make follow-up exercise far more effective.
For patients dealing with ongoing muscle guarding, this often works best when paired with a broader rehab approach such as physical therapy for chronic muscle tightness, where the goal is not only to release a painful area but also to address why it keeps returning.
What dry needling does not do
It doesn’t magically fix every pain problem in one visit. It doesn’t replace strengthening. And it doesn’t mean the body is broken in some mysterious way.
Dry needling is most useful when a muscle is contributing to pain, stiffness, or poor movement. That’s why a proper physical therapy assessment matters so much. The therapist has to decide whether the painful area is the driver, a compensation, or both.
Common Conditions Treated with Dry Needling
Some patients hear “dry needling” and think it’s only for a sore neck or upper back knot. In practice, therapists use it for a much wider range of musculoskeletal problems when trigger points, guarding, or pain-sensitive tissues are part of the picture.

Back pain and sciatica
A common example is low back pain that feels deep, stubborn, and hard to stretch out. Sometimes the painful muscles are in the low back itself. Other times, the primary driver is in the glutes, hip rotators, or hamstrings. Those areas can stay tight and protective, especially after lifting injuries, long periods of sitting, or compensation after a flare-up.
Sciatic symptoms can be especially confusing. Not every case of pain down the leg comes only from the spine. Muscles in the hip and pelvis can also contribute to radiating discomfort, tension, and movement restriction. Dry needling may help reduce that muscular component so walking, bending, and strengthening work become more tolerable.
Neck pain and shoulder problems
Desk workers often come in with a familiar pattern. The upper traps are always tense. Turning the head feels limited. Headaches may start near the base of the skull. In these cases, trigger points in the neck, upper back, and shoulder girdle can keep the area in a cycle of pain and guarding.
Shoulder pain works the same way. A patient with rotator cuff irritation or tendon overload may also have protective tension in the deltoid, infraspinatus, pecs, or upper back. Needling those areas can reduce the “bracing” response so shoulder mechanics improve during rehab.
Sports injuries and overuse problems
Athletes often describe one area that never quite resets. A calf that stays tight after a strain. A quad that keeps pulling. A forearm that won’t calm down after repetitive gripping. Dry needling can be helpful when overworked tissue keeps limiting speed, power, or recovery.
Here are a few patterns therapists commonly look for:
- Post-strain guarding: A healed muscle still acts threatened and stays tight.
- Compensatory overload: One region is working too hard because another is weak or stiff.
- Pain with return to sport: Motion is technically available, but pain still changes mechanics.
Muscles don’t need to be torn to be a major pain source. Sometimes they just stay switched on for too long.
An important but less discussed use
Dry needling is also being used in pelvic health. According to ChoosePT’s overview of dry needling, an underserved application is for pelvic floor disorders, including issues affecting 25% to 50% of postpartum women, such as overactive pelvic floor muscles causing pain and underactivity contributing to stress leakage. That use expands the conversation well beyond back and neck pain.
The larger lesson is simple. Dry needling isn’t tied to one body part. It’s tied to whether irritated muscles and connective tissue are part of the problem.
Dry Needling vs Acupuncture What Is the Difference
This is the question almost every patient asks. The confusion makes sense because both treatments use very thin needles. But the purpose, framework, and clinical reasoning are different.
Dry needling is based on modern anatomy, biomechanics, and neurophysiology. The therapist evaluates muscles, trigger points, movement restrictions, and pain patterns, then chooses specific tissues to treat. Acupuncture comes from Traditional Chinese Medicine and uses a different framework for diagnosis and treatment.
If you’re already curious about acupuncture in a separate context, this explanation of how acupuncture works for fertility is a helpful example of how acupuncture is discussed through its own treatment model rather than a physical therapy trigger-point model.
Dry Needling vs. Acupuncture at a Glance
| Aspect | Dry Needling | Acupuncture |
|---|---|---|
| Origin | Modern Western rehabilitation and musculoskeletal care | Traditional Chinese Medicine |
| Primary goal | Reduce pain and improve movement by targeting trigger points and dysfunctional muscle tissue | Address symptoms through a Traditional Chinese Medicine framework |
| Assessment style | Physical therapy exam based on anatomy, movement, tissue irritability, and function | Acupuncture evaluation based on its own diagnostic model |
| Typical target | Myofascial trigger points, painful muscle bands, movement-limiting tissues | Points selected according to acupuncture principles |
| How patients often describe the purpose | “Loosen the tight area so I can move and rehab better” | “Support balance and symptom relief using acupuncture methods” |
Why the difference matters to patients
For a patient, the biggest practical difference is the treatment goal. If your issue is a painful calf trigger point after running, a tight piriformis contributing to sciatic symptoms, or neck muscles restricting rotation, dry needling is used as part of a physical therapy plan focused on movement and function.
If you want to compare approaches for pain care more broadly, some clinics also offer acupuncture for pain relief. The right option depends on your diagnosis, goals, and which treatment model fits your needs.
Your First Dry Needling Session What to Expect
People are often less worried about the treatment itself than the unknown. Once they know what the appointment looks like, the anxiety usually drops.

It starts with an exam, not a needle
A good dry needling session begins with clinical reasoning. The therapist asks where the pain is, what movements aggravate it, when it started, and whether the involved tissues fit a dry needling approach. They’ll also check movement, strength, sensitivity, and tissue tension.
That matters because not every painful spot should be needled. Sometimes the area that hurts is compensating for another problem. Sometimes exercise or hands-on mobilization is the better starting point. If you’ve never been through rehab before, this overview of what a typical physical therapy session looks like can make the whole process feel more familiar.
During the treatment
The therapist cleans the area and uses sterile, single-use needles. Many patients are surprised that insertion often feels minimal. The stronger sensation, if it happens, is usually the local twitch response or a deep ache in the muscle.
Common sensations include:
- A quick twitch: The muscle jumps briefly.
- A deep crampy feeling: Often short-lived and very specific to the tight spot.
- Pressure or heaviness afterward: The area may feel worked on, similar to deep manual therapy.
Some needles are inserted and removed quickly. Others may stay in briefly depending on the treatment style and body region.
A short visual walk-through can also help if you’re more comfortable seeing the process first.
After the needles come out
Most patients get up and move right away. The therapist may have you recheck a motion that was painful before, then follow treatment with corrective exercises or mobility work.
Practical rule: Dry needling usually works best when you use the new motion right away. That’s how the body learns the safer pattern.
It’s also normal to feel post-treatment soreness. Many people compare it to the soreness after a tough workout or deep tissue work. That doesn’t mean something went wrong. It usually means the tissue and nervous system got a strong input.
Is Dry Needling Safe and Effective
Patients usually want straight answers here. Does it work, and is it safe enough to try?
What the research supports
According to the Federation of State Boards of Physical Therapy dry needling report, research shows dry needling is more effective for reducing pain and improving pain pressure threshold compared to sham or no treatment. The same analysis found statistically significant effects on pain reduction and functional outcomes in the immediate to 12-week follow-up period. It also reported that when compared with first-line approaches such as NSAIDs, topical creams, ice, and bracing, dry needling was equally effective at 3 months and significantly superior at 6 months.

That’s encouraging, but it also helps to be realistic. The same body of evidence suggests the clearest benefits are short-term. In practice, that’s often exactly what rehab needs. A short-term drop in pain can create room for long-term gains through strength, mobility, and improved movement patterns.
What patients usually notice
When dry needling is a good fit, patients commonly report:
- Less pain with movement: Turning, bending, lifting, or walking feels easier.
- Reduced muscle guarding: The body stops bracing so hard around the painful area.
- Better tolerance for exercise: Strengthening and mobility work become more productive.
That combination matters more than any single symptom change. The ultimate goal is using pain relief to restore normal function.
Safety and side effects
Dry needling is considered safe when performed by a properly trained clinician using appropriate screening, sterile technique, and sound anatomical knowledge. Still, “safe” doesn’t mean “nothing is felt.”
Typical short-term reactions include mild soreness, a small bruise, temporary fatigue, or a little local bleeding at the insertion site. Those responses are generally manageable and brief. A good therapist also screens for situations where dry needling may not be appropriate, such as certain medication issues, infection concerns, or strong needle anxiety.
The safest treatment is the one matched to the right patient, the right tissue, and the right point in recovery.
That’s why the decision should come after an evaluation, not before it.
Start Your Recovery at MedAmerica Rehab Center
If your back tightens every time you get out of the car, your neck locks up by the end of the workday, or sciatica keeps sending pain down your leg, it helps to have a plan that looks at the whole problem, not just the sore spot.
Dry needling can play a useful role in that plan. It may help relax an overactive muscle and make movement easier, but the ultimate goal is what comes next. Once pain eases, your therapist can help you retrain how the area moves, build strength where support is missing, and correct the habits that keep the problem returning.
That matters for the conditions MedAmerica treats every day.
At MedAmerica Rehab Center, care is built around the reason your pain started and the reason it has stayed. For one patient, that may mean dry needling plus core and hip work for ongoing low back pain. For another, it may mean easing tight neck muscles so posture training and shoulder mechanics finally start to stick. Athletes often need the same kind of step-by-step approach. Calm the irritated tissue, restore normal motion, then rebuild power and control so the injury is less likely to flare up again.
The same idea applies if you have sciatica, a sports injury, arthritis, are recovering after surgery, or are healing after an accident. Dry needling is one tool. Your recovery plan may also include hands-on therapy, guided exercise, mobility work, and practical changes for daily activities.
Since 1995, the team in Deerfield Beach has focused on patient-centered care that helps people return to daily life with less pain and better function. If you are unsure whether dry needling fits your situation, start with an evaluation. A good assessment should answer two questions clearly: Can this treatment help, and what else does your body need to recover well?
Frequently Asked Questions About Dry Needling
Does dry needling hurt
The sensation is often reported as more strange than painful. The needle itself is often barely felt. The stronger sensation is usually the twitch or deep ache in the tight muscle, and that usually passes quickly.
How many sessions will I need
That depends on the condition, how long you’ve had it, and whether muscle trigger points are the main driver of pain. Some people notice change quickly. Others need repeated treatment as part of a broader physical therapy plan.
Is dry needling the same as getting a shot
No. Nothing is injected. That’s why it’s called “dry” needling. The needle is used to stimulate tissue, not deliver medication.
Will I still need exercises if I do dry needling
Usually, yes. Dry needling may reduce pain and tension, but exercise helps your body keep the gains. That’s especially important for back pain, neck pain, sciatica, and sports injuries.
Is dry needling covered by insurance
Coverage varies by plan and provider. The best next step is to ask the clinic and your insurance company what your policy includes for physical therapy and dry needling services.
If you’re dealing with persistent back pain, neck tension, sciatica, or a sports injury that won’t fully settle down, MedAmerica Rehab Center can help you figure out whether dry needling belongs in your recovery plan. Their team serves Deerfield Beach with individualized care that combines physical therapy, hands-on treatment, and clear guidance so you can feel better, move better, and get back to the activities you enjoy.

