How to Prevent Falls at Home: A Practical Safety Plan
A lot of people start thinking seriously about falls after a close call. Maybe you caught yourself on the bathroom counter. Maybe your parent says they're “fine,” but they've started using furniture to steady themselves. Maybe pain in your back, knee, or hip has made ordinary movements feel less automatic than they used to.
That's usually the moment when the question changes. It stops being “Should I be worried?” and becomes “How do I make home safer without making life harder?” That's the right question.
The best fall-prevention plans don't rely on one fix. They combine safer spaces, better movement habits, stronger balance, and honest attention to the physical limits that come with arthritis, sciatica, surgery recovery, or general stiffness. If you're trying to figure out how to prevent falls at home for yourself or someone you love, start with practical changes you can use right away.
Why Fall Prevention Is More Than Just Tidying Up
Many homeowners think fall prevention means picking up clutter and removing a rug or two. That helps, but it's only part of the picture. A fall usually happens when personal risk factors and home hazards meet at the same time.
The Centers for Disease Control and Prevention reports that more than 1 in 4 older adults falls each year, and falling once doubles the chance of falling again. The CDC also points to common household contributors such as broken or uneven steps, throw rugs, and clutter, while noting that prevention also involves lighting, footwear, and vision issues. That's why a better approach is to reduce several risks at once, not just one of them (CDC fall facts and home risk factors).

The home matters, but so does the body moving through it
A clear hallway won't fully protect someone who gets dizzy when standing up. A grab bar won't solve the problem if leg weakness makes it hard to rise from a chair. And even a well-organized kitchen can still be risky for someone recovering from surgery who can't twist, bend, or pivot safely.
That's why I encourage people to stop treating falls as a housekeeping problem. It's a mobility problem, a pain problem, a balance problem, and often a timing problem too. People fall when they rush to the bathroom at night, reach for something awkwardly, turn too quickly, or try to move the way they used to move before pain changed their mechanics.
Practical rule: If a task feels harder because of pain, weakness, stiffness, or recent surgery, it's also more likely to become a fall risk.
Prevention protects independence
Some people resist making changes because they think it means “giving in.” In reality, fall prevention is one of the most practical ways to stay independent. It keeps daily routines realistic. It also lowers the mental load that comes from feeling unsteady in your own home.
A good plan isn't about making the house look medical. It's about making ordinary tasks more forgiving. You want fewer slippery decisions, fewer rushed turns, fewer low seats that are hard to get out of, and fewer moments where balance has to be perfect.
Here's the mindset that works best:
- Reduce friction: Make the safe choice the easy choice.
- Match the setup to the person: A home that works for an active adult may not work for someone with sciatica, arthritis, or recent joint surgery.
- Fix clusters, not single hazards: Better lighting plus safer footwear plus a cleared path is stronger than any one change alone.
When people ask how to prevent falls at home, the answer isn't “be more careful.” It's change the environment and the way you move through it.
Your Room-by-Room Home Safety Makeover
The fastest way to improve safety is to walk through the home and look at each room with fresh eyes. Don't ask, “Does this room seem fine?” Ask, “What happens here when I'm tired, stiff, in pain, carrying something, or moving at night?”
Research on home modification shows that targeted changes can make a real difference. A Washington University School of Medicine report described a community-based in-home program that reduced harmful in-home falls by nearly 40% after occupational therapists recommended changes such as grab bars, shower seating, slip-resistant bathroom surfaces, better lighting, and stair handrails (Washington University School of Medicine home modification findings).
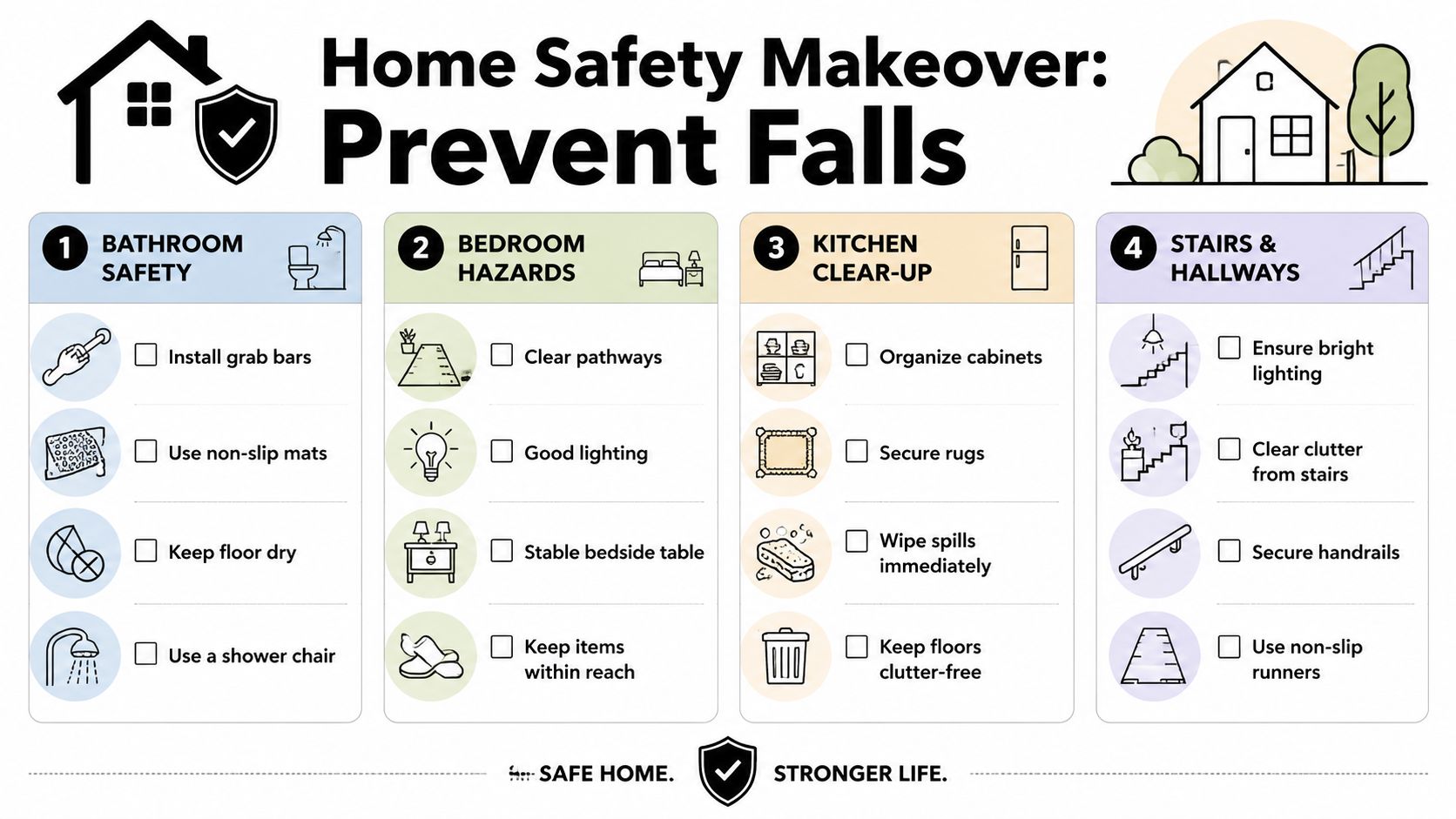
Bathroom
The bathroom is where small movement problems become obvious. Wet floors, quick turns, low toilet seats, and stepping over a tub wall all demand control. If you have back pain or knee stiffness, this room can become risky even when it looks clean.
Use this checklist:
- Install real grab bars: Place them where your hand naturally wants support, usually near the toilet and inside or just outside the shower entry. Towel bars aren't built to hold body weight.
- Add shower seating: A shower chair or bench helps when standing for several minutes increases pain or fatigue.
- Improve traction: Use slip-resistant mats or adhesive strips inside the shower, and keep the outer floor dry.
- Raise what's too low: A raised toilet seat can make transfers much safer if squatting down and standing up is difficult.
- Simplify the setup: Keep soap, shampoo, and towels within easy reach so you don't have to twist or bend suddenly.
If stepping into the tub is hard, don't force a high, awkward leg lift while holding a wet shower curtain. Pause, hold support, and move one step at a time.
Bedroom
Many falls happen during ordinary moments in the bedroom. Getting up too quickly, walking in dim light, or navigating around furniture when sleepy can turn a routine trip to the bathroom into a dangerous one.
Focus on the path from bed to door.
- Clear the walking lane: Remove baskets, shoes, cords, and decorative stools from the route.
- Set up reachable lighting: A lamp or switch should be easy to reach from bed.
- Choose stable furniture: A sturdy nightstand is useful. A lightweight table that slides when touched is not.
- Check bed height: You should be able to sit with your feet planted firmly before standing.
- Keep essentials nearby: Glasses, phone, medications, and water should be close enough that you don't have to lunge or overreach.
If you have pain or post-surgery restrictions, take a moment at the edge of the bed before standing. Let your body catch up before your feet start moving.
Kitchen
The kitchen encourages multitasking, and that's part of the danger. People twist while carrying plates, reach overhead for cookware, and hurry across slick spots without noticing them.
A safer kitchen usually comes down to layout.
- Bring daily items to waist or chest height: Store dishes, mugs, pans, and frequently used food where you can reach them without a stool.
- Wipe spills right away: Even a small splash near the sink can become a sliding hazard.
- Secure or remove rugs: If a rug shifts or curls, it's not worth keeping.
- Avoid carrying too much at once: One safe trip beats one rushed trip with blocked vision.
- Create turn space: If you use a cane or walker, make sure the path between counter, sink, refrigerator, and table isn't cramped.
For people with back pain, the problem often isn't just the floor. It's repeated bending into low cabinets. Move heavy pots, pet food, and cleaning supplies higher if possible.
Stairs and hallways
Stairs punish hesitation and poor visibility. Hallways create problems when they're dim, crowded, or used as storage.
Here's what to inspect:
| Area | What to check | Better option |
|---|---|---|
| Stairs | Loose railings, poor grip, dark steps | Secure handrails and brighter lighting |
| Step edges | Hard-to-see transitions | Increase contrast and improve visibility |
| Hallways | Cords, décor, small tables, clutter | Keep a wide clear route |
| Entry areas | Shoes piled near doors | Use organized storage off the walking path |
If your stair lighting is weak, adding dedicated illumination can help you see each edge clearly. This guide on how to install step lights gives a useful overview of what to consider before upgrading.
What works and what doesn't
Some fixes consistently help. Others only create the appearance of safety.
Usually worth doing
- Grab bars in the right places
- Shower seating for low endurance or poor balance
- Handrails that feel solid
- Brighter lighting on routes used at night
- Removing unstable rugs and clutter
Often overrated or poorly done
- Using furniture as support instead of proper rails or bars
- Keeping a pretty rug that still slides
- Buying equipment without checking if it fits the person
- Making changes in one room while ignoring the route to that room
A safe room doesn't help much if the path to it is still risky.
Essential Habits for Safe Movement
A safer home works best when your daily habits support it. However, maintaining these habits can be a challenge. They install a grab bar, then keep wearing slippery socks. They clear the hallway, then walk it in the dark. They buy a cane, then leave it leaning in the wrong room.

Wear footwear that helps instead of hinders
Indoor falls often start at the feet. Socks slide. Backless slippers drift. Shoes that are soft and comfortable but unstable can make turning and weight shifting harder, especially on tile or polished floors.
Look for footwear with:
- A closed back: So the shoe stays on during turning
- A non-slip sole: Good traction matters indoors too
- A secure fit: Not tight, but not loose
- Enough support: The foot shouldn't wobble inside the shoe
If pain makes it hard to put shoes on, choose a pair that's easy to manage but still stable. Convenience matters, but not at the cost of traction.
Make light part of the routine
Good lighting is a movement tool. It helps your brain judge distance, edges, and obstacles before your foot lands. That matters even more if you already feel stiff, cautious, or unsteady.
Use light proactively:
- Turn lights on before moving, not halfway through the trip.
- Place nightlights on the route to the bathroom and any hallway used after dark.
- Reduce glare if bright reflections make surfaces harder to judge.
- Keep switches accessible so you don't cross a dark room to find one.
Better lighting doesn't just help you see the hazard. It gives you more time to respond to it.
Use assistive devices correctly
A cane or walker can make movement safer, but only if it fits the person and is used consistently. The common mistake is waiting too long to use one, or using one that's the wrong height.
Consider an assistive device if you notice any of these patterns:
- You reach for walls or furniture while walking
- Turning feels shaky
- Pain causes you to unload one leg
- You avoid certain rooms because the walk feels uncertain
A device shouldn't make you feel trapped or older. It should make your gait more predictable. The right setup can reduce sudden weight shifts, especially when pain flares or fatigue sets in late in the day.
There's another habit that matters just as much. Don't rush transitions. Pause before standing. Turn in small steps instead of pivoting sharply. Hold support before lifting a foot over a threshold. Those simple habits are often the difference between a near miss and a fall.
Building a Stronger and Steadier You
Home changes reduce risk, but your body still needs enough strength and control to use those spaces well. When the legs are weak or balance reactions are slow, everyday movements become more demanding. Standing from a chair, turning in the kitchen, and stepping into the shower all require more than people realize.

Start with controlled, supported practice
You don't need complicated equipment to begin. You do need a stable surface, good shoes, and enough honesty to stop before you become unsafe. If any exercise increases sharp pain, dizziness, or a strong sense that you might lose balance, stop and get guidance.
A few simple exercises help many people:
Sit-to-stands
This builds leg strength for one of the most common daily tasks.
- Sit in a firm chair.
- Place your feet under you.
- Lean forward slightly from the hips.
- Stand up using as little hand support as you safely can.
- Sit back down with control.
If you have knee pain or recent surgery, use a higher chair at first. The goal is smooth control, not speed.
Counter-supported heel raises
This helps with ankle strength and balance control.
- Stand at a kitchen counter and hold lightly.
- Rise up onto your toes.
- Pause briefly.
- Lower slowly.
This movement supports steadier walking and can improve push-off during gait.
Marching in place with support
This is useful for balance and weight shifting.
- Stand tall at a counter.
- Lift one knee, then the other.
- Move slowly enough that you stay in control.
- Avoid leaning heavily onto your hands.
People with hip stiffness often do better with smaller lifts at first.
A more detailed home routine can help if you want structured progression. MedAmerica Rehab provides guidance on fall prevention exercises for seniors, including balance and strength work that can be adapted to different mobility levels.
Practice movement quality, not just repetition
The way you move matters as much as the number of reps. A rushed sit-to-stand with poor foot placement won't teach stability. A controlled one will.
“Slow and steady” is useful advice only if you also move with good setup, good support, and good attention.
Another helpful drill is tandem standing, sometimes called heel-to-toe standing.
- Stand near a counter.
- Place one foot slightly in front of the other.
- Hold the counter as needed.
- Maintain your balance for a short period, then switch sides.
This challenges balance in a narrow base of support, which is often where people feel unsteady during turns or when navigating tight spaces.
Here's a short demonstration for additional guided movement practice:
Match the exercise to the problem
If getting out of a chair is hard, train that movement. If turning is your weak spot, practice small controlled turns with support nearby. If shower entry feels risky, work on step control and single-leg stability under supervision.
The best exercise plan is specific. It respects pain, accounts for recovery limits, and builds confidence without asking you to “push through” movements that aren't safe yet.
Managing Your Health for Better Stability
Falls rarely come from one cause. A person may have mild balance loss, a sedating medication, poor depth perception in dim light, and morning stiffness all at once. That combination is why broad health management matters.
A 2024 World Health Organization report continues to emphasize that falls are the second leading cause of unintentional injury death worldwide, and older adults need individualized strategies that combine environmental changes with balance and strength support, not home fixes alone. The National Institute on Aging also frames prevention in practical home terms, which fits what clinicians see every day: falls are multifactorial, especially for people dealing with pain, stiffness, or recovery (National Institute on Aging guidance on preventing falls at home).
Review medications with a purpose
Many people accept dizziness, grogginess, or feeling “off” as a normal trade-off for treatment. It isn't something to ignore. If a medicine affects alertness, blood pressure, coordination, or reaction time, it can change how safely you move through your home.
Bring specific observations to your doctor or pharmacist:
- When do you feel lightheaded
- Do you feel unsteady after taking a certain medication
- Do symptoms worsen when you first stand up
- Are you more foggy at night
That conversation is much more useful than saying, “I don't feel great.”
Don't wait on vision changes
Vision affects much more than reading. It helps you judge depth, detect edges, and adjust to flooring changes. Small visual changes can create big movement errors, especially on stairs or in bathrooms with shiny surfaces.
If you've started misjudging step height, reaching inaccurately, or feeling less sure in dim spaces, schedule an eye exam. It's also smart to check whether your most-used areas of the home match your current visual needs.
Have a plan for a bad day
People often prepare the house but never prepare for what happens if a fall still occurs. That leaves them more fearful than they need to be.
A simple emergency plan can include:
- Keeping a phone within reach
- Telling family or neighbors if balance has recently worsened
- Using an alert device if you spend long periods alone
- Practicing how to pause and call for help rather than rushing to get up
For people whose walking has changed after surgery, pain, or deconditioning, focused mobility work often matters as much as home setup. That's where gait training in physical therapy can be useful, because it addresses how you walk, turn, transfer, and recover your balance during real movement.
When You Need a Partner in Prevention
There's a point where do-it-yourself changes stop being enough. If you've already fallen, nearly fallen several times, or started avoiding normal activities because you don't trust your balance, it's time for a more structured assessment.
The strongest fall-prevention workflows don't rely on guesswork. In one home-based program, a physical or occupational therapist completed a 60 to 90 minute visit that included functional testing such as the Timed Up and Go test, along with an in-home hazard review. That kind of multifactorial approach matters because it looks at mobility, transfers, lower-extremity power, and the environment together. In that study, the program led to a 23.9% relative reduction in falls (multifactorial home fall-prevention assessment study).
Signs you shouldn't ignore
Professional help makes sense when any of these are true:
- A recent fall changed your confidence
- You feel unsteady during turns or transfers
- Pain has altered how you walk
- You've had surgery and still don't trust your movement
- Family members notice you grabbing furniture or slowing down noticeably
A proper evaluation can identify whether the main problem is strength, gait mechanics, reaction time, poor transfer technique, home setup, or a mix of all of them.
What a structured program should include
Look for a program that goes beyond generic exercise sheets. It should include functional testing, movement analysis, and practical recommendations that fit your actual home and routine. One option is a formal fall risk assessment for elderly adults, which can help clarify where the risk is coming from and what to address first.
For many people, the biggest relief is finally understanding why they feel unsafe. Once you know whether the issue is balance, pain, weakness, turning, or transfer control, the next steps become much clearer.
If you or someone you love is feeling less steady at home, MedAmerica Rehab Center can help you take the next practical step. Our team works with people dealing with pain, post-surgical recovery, balance problems, and walking changes, with care plans focused on safer movement and everyday function.

