Sports Injury Physiotherapy: Recover Fast & Get Back in Play
You felt it again on the second mile. Or in the third set. Or the morning after a game when your shoulder reminded you that throwing, serving, or reaching overhead still isn't right.
At first, most active people do the same thing. They stretch a little more, ice it, rest for a few days, then get back to training. The pain fades just enough to be ignored. Then it returns. Same spot. Same frustration. Sometimes worse.
That cycle is where sports injury physiotherapy matters most. Not when an injury is dramatic and obvious, but when it becomes a pattern. The runner with recurring knee pain. The pickleball player whose shoulder aches after every match. The gym-goer whose ankle never felt stable again after "just a sprain." These problems often linger because the body part that hurts isn't always the underlying source of the problem.
That Nagging Injury That Just Wont Go Away
A familiar story walks into clinic all the time. Someone says, "My knee keeps flaring up when I run, so I've been foam rolling my quad and taking a few days off." That sounds sensible. Sometimes it even helps for a week or two.
Then the pain returns because the knee was only the messenger.
A sore knee may reflect a hip that isn't controlling the leg well. A painful shoulder may be reacting to poor ribcage position, stiff upper back motion, or a loss of control in the shoulder blade. An ankle that keeps rolling may never have regained balance, timing, and confidence after the first sprain. When treatment stays glued to the painful area, recovery often stalls.
Pain has a location, but movement has a pattern
Many active adults encounter a common pitfall: they search by body part. Knee stretches. Shoulder exercises. Ankle brace. Those tools can help, but they're incomplete when nobody has asked the bigger question: why is that tissue being overloaded in the first place?
Two runners can both say they have knee pain and need completely different solutions. One may have limited ankle mobility and overload the knee on every stride. Another may have weak hip control and let the thigh collapse inward during landing. The symptom sounds identical. The fix isn't.
The body works like a chain. If one link stops doing its job, another link pays for it.
That same logic applies to training habits. If your schedule swings between too much and too little, tissues don't adapt well. If you're trying to train hard without enough recovery, these injury-free workout strategies are worth reviewing because they address the habits that often keep small problems alive.
Temporary relief is not the same as recovery
Many people have already tried some version of self-treatment before they seek help:
- Rest alone: It can calm irritation, but it usually doesn't rebuild capacity.
- Random online exercises: They may be good exercises, just not the right ones for your mechanics.
- Pain-masking approaches: They can reduce symptoms short term while leaving the movement fault untouched.
Lasting progress starts when someone looks beyond the sore spot and studies how you move under functional load. That's where the underlying answers usually show up.
The True Goal of Sports Physiotherapy
Sports injury physiotherapy isn't just about getting you out of pain. That's part of it, but it isn't the finish line.
A better way to think about it is this. A good sports physiotherapist works like a high-performance mechanic. If a warning light turns on in a car, the job isn't to cover the light with tape and send the driver back onto the road. The job is to find out what's causing the warning in the first place, fix it, then make sure the system can handle speed again.
Your body deserves the same standard.
First, calm the irritated tissue
When an injury is fresh or flared up, you need to settle things down enough to move well again. That may mean reducing pain, easing protective muscle tension, and restoring enough motion that daily life and light training don't keep provoking the area.
This phase matters because people often do one of two unhelpful things:
- Push too soon: They test the injury every day and keep re-irritating it.
- Shut down completely: They avoid movement so long that stiffness, weakness, and fear start driving the problem.
The right approach usually sits in the middle. Protect what's irritated, but keep the body moving in ways it can tolerate.
Then, rebuild what the injury exposed
Most injuries reveal a weak point. Not a character flaw. A physical weak point.
Sometimes it's strength. Sometimes it's mobility. Sometimes it's motor control, which is your body's ability to put force in the right place at the right time. Rehab then becomes active. We don't just ask, "Does it hurt less?" We ask better questions.
- Can the joint move through the range your sport demands?
- Can the muscles produce force without compensation?
- Can you control that force on one leg, under speed, fatigue, or direction change?
If the answer is no, the tissue may feel quieter, but the athlete isn't ready.
Practical rule: If treatment only makes pain smaller but doesn't make movement better, you're not done.
Finally, make re-injury less likely
The best sports rehab doesn't return you to the exact setup that got you hurt. It changes that setup.
That means correcting loading errors, improving movement efficiency, and preparing the body for the specific demands of your sport or activity. A tennis player needs different movement qualities than a runner. A recreational basketball player needs something different than someone recovering for weekend golf. The tissue may be the same. The return target is not.
Three outcomes matter most in a strong rehab plan:
- Symptoms improve enough for consistent progress
- Strength, mobility, and control return where they need to
- Your movement pattern becomes more durable under real-life sport demands
That last piece is what separates basic injury care from true sports injury physiotherapy. Pain relief is the opening chapter. Resilience is the ending you want.
Common Sports Injuries and Why They Happen
Some body regions take more punishment than others in sport. In a study of athletes in physical therapy, the knee was the most commonly injured site at 30.09%, followed by the shoulder at 22.69% and the ankle at 20.37%. The same study reported that 86.11% had significant pain reduction after physiotherapy, 63.89% returned to sport, and the re-injury rate was 8.80% according to this sports physiotherapy outcomes study.
Those numbers line up with what clinicians see every week. Knees, shoulders, and ankles tend to absorb the consequences when strength, timing, mobility, and technique drift off course.

Knee injuries
Knee pain is common because the knee often sits in the middle of the problem. It handles force from the ground below and control from the hip above. When either side does its job poorly, the knee takes extra stress.
That shows up in several familiar patterns:
- Front-of-knee pain: Often linked to poor control when squatting, running, or descending stairs.
- Ligament sprain patterns: Often tied to cutting, pivoting, or landing mechanics.
- Tendon overload: Common when training volume rises faster than tissue capacity.
A knee complaint may start at the knee, but it doesn't always stay there diagnostically. Limited ankle motion can force the knee to move in ways it doesn't like. Weak hip stabilizers can let the leg collapse inward under load. Trunk control matters too. If the pelvis and torso drift, the knee pays for it.
Shoulder injuries
Shoulders are built for mobility, which is both their gift and their vulnerability. In overhead sports and gym training, the shoulder has to move freely while staying centered and controlled.
When that balance slips, athletes often deal with:
- Rotator cuff irritation
- Impingement-style pain
- Tendon overload with pressing, serving, or throwing
The root issue is often not "a bad shoulder" in isolation. Poor shoulder blade mechanics, stiff upper back motion, and weak force transfer from the trunk can all change how the shoulder loads. The person feels pain at the top or front of the shoulder, but the underlying issue may involve the entire chain that supports overhead motion.
Ankle injuries
Ankles get written off too easily. Someone rolls it, swells up, rests, then returns once they can tolerate activity again. That often leaves the job half done.
What follows can include:
- Repeated sprains
- A sense of instability on uneven ground
- Reduced confidence when landing or changing direction
An ankle sprain isn't just about loosened tissue. It can also disturb balance, body awareness, timing, and lower-leg strength. If those pieces don't recover, the athlete starts guarding, altering stride, or shifting load upward to the knee and hip. That's one reason thorough ankle injury recovery care should look at more than swelling and range of motion.
Common Sports Injuries at a Glance
| Injury Area | Common Causes in Athletes | Initial Physiotherapy Focus |
|---|---|---|
| Knee | Poor landing mechanics, weak hip control, limited ankle mobility, training overload | Calm irritation, restore motion, improve single-leg control and force alignment |
| Shoulder | Repetitive overhead loading, poor shoulder blade control, stiff upper back, weak trunk support | Reduce pain, restore mobility, retrain shoulder blade and rotator cuff control |
| Ankle | Awkward landing, cutting or pivoting, incomplete rehab after sprain, balance deficits | Control symptoms, rebuild stability, restore balance and confidence under load |
A diagnosis names the injured tissue. A movement assessment explains why that tissue got overloaded.
That difference matters. It's how treatment stops being a patch and starts becoming a plan.
Your Comprehensive Physiotherapy Assessment
The first appointment shouldn't feel like guesswork. It should feel like someone is building a map.
A thorough sports injury physiotherapy assessment starts with your story, but it doesn't stop there. We want to know what happened, when it hurts, what you've already tried, and what you're trying to get back to. Running a comfortable three miles is different from cutting hard on a soccer field. Returning to lifting overhead is different from sleeping without pain. Your goals shape the plan.
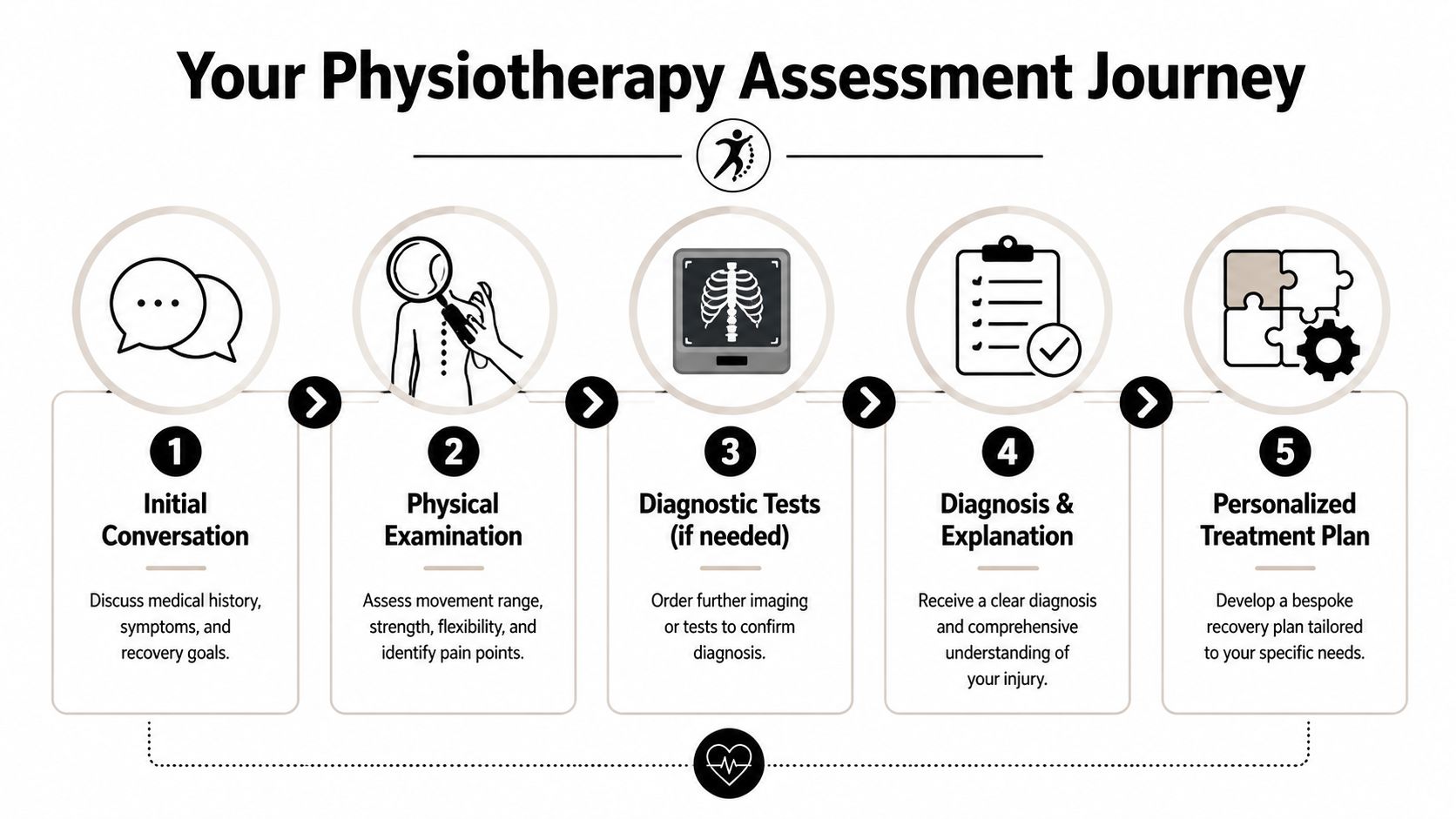
What happens in the room
Once the conversation is clear, the physical exam begins. At this point, a lot of patients realize that a sports assessment is much more detailed than "tell me where it hurts."
A strong exam often includes:
- Movement testing: Squat, step-down, lunge, reach, push, pull, or sport-specific patterns.
- Range of motion checks: Not just whether a joint moves, but how cleanly it moves.
- Strength testing: Looking for force deficits and side-to-side differences.
- Palpation and tissue exam: Finding tender structures, stiffness, or protective guarding.
- Balance and control tasks: Especially after ankle, knee, and hip injuries.
These tests matter because symptoms can be misleading. A runner with knee pain may not have a knee problem first. The issue may begin with a stiff ankle that blocks proper loading, or with a hip that doesn't control the thigh when the foot hits the ground. You don't find that by asking where it hurts once and handing over a generic band exercise.
Why biomechanics changes the whole picture
Advanced biomechanical analysis can go much further than the naked eye. Some systems use high-speed cameras and force plates to capture movement details that standard observation misses, helping therapists identify asymmetries and dysfunctions and build a precise rehab plan through data-driven biomechanical analysis.
In simple terms, this means we can study how force travels through your body instead of just looking at the sore spot.
Consider it this way:
- A video replay shows what happened.
- Force data helps explain why it happened.
- Movement analysis tells us what to retrain.
A jump test may reveal that one leg isn't accepting load well. A landing assessment may show delayed control through the hip. A change-of-direction test may expose why the ankle keeps feeling untrustworthy. These are the details that turn rehab from broad advice into specific correction.
When a movement fault is subtle, the body still feels it even if the eye misses it.
The kinetic chain matters
The body doesn't perform sport one joint at a time. It works as a connected system, often called the kinetic chain. If one segment loses mobility or control, another segment usually compensates.
That is why assessment may include areas that seem unrelated to your pain:
- Foot and ankle mechanics for someone with knee irritation
- Thoracic spine and shoulder blade motion for someone with shoulder pain
- Hip control and trunk stability for both running and cutting athletes
Patients are often surprised by this. They expect treatment to stay at the painful site. But if the chain is the problem, local treatment alone won't hold.
What you should leave with
A useful first visit ends with clarity. You should understand:
- What tissue is irritated
- What movement or loading issue may be contributing
- What aggravates it and what helps
- What the first phase of treatment will focus on
- What progress will need to look like before return to full sport
That last part matters. Recovery should not be based on hope or on one good day. It should be based on whether your body can repeatedly tolerate the tasks your sport demands.
A careful assessment doesn't slow recovery down. In most cases, it keeps people from wasting weeks on the wrong plan.
Your Personalized Treatment Toolkit
Once the assessment identifies the underlying problem, treatment gets much more focused. Good sports injury physiotherapy uses a toolkit, not a single favorite method. Each tool has a job. The key is using the right one at the right time.

Manual therapy for mobility and symptom relief
Manual therapy is one of the most valuable tools when a joint feels blocked, a muscle is guarding, or pain is making normal motion hard. The simplest analogy is a skilled craftsperson freeing up a stuck hinge so the door can swing the way it was designed to.
That can include hands-on work aimed at:
- Improving joint mobility
- Reducing protective muscle tension
- Helping painful movement feel safer and smoother
This approach isn't fringe care. During the Rio Olympic Games, physiotherapy services delivered 3,539 procedures, and manual therapy made up 27.5% of treatments in this Olympic physiotherapy report. At that level, nobody wastes time on techniques that don't have a practical role.
Manual therapy works best when people understand its limits. It can create a useful window. It can reduce stiffness and pain. It usually does not hold long term if nobody follows it with the strength and control work that teaches the body to keep the change.
Therapeutic exercise is the center of rehab
If manual therapy opens the door, therapeutic exercise teaches the body how to walk through it.
This is the part patients need most, even though it's not always the part they expect to value most at the start. Exercise restores capacity. It rebuilds tissues so they can tolerate force again. It retrains motor control so your body uses that force in a better pattern.
A smart exercise program usually progresses through stages:
| Phase | What it targets | What it may feel like |
|---|---|---|
| Early phase | Pain-free activation, gentle mobility, restoring confidence | Controlled, simple, often slower than expected |
| Middle phase | Strength, endurance, single-leg control, tolerance to load | More challenging, but still deliberate |
| Return phase | Plyometrics, direction changes, sport-specific demands | Closer to real sport effort and speed |
This is also where simple recovery tools can support the process. Some patients benefit from short-term symptom management with cold application between sessions. If you're using icing at home, this guide on using an ice pack in physical therapy gives a practical overview of when it helps and where people tend to overuse it.
Advanced options for stubborn injuries
Some injuries don't respond well to exercise alone, especially when a tendon has stayed irritated for a long time or the area remains very sensitive. In those cases, advanced modalities may help move things forward.
Shockwave therapy
Shockwave therapy is often used for chronic tendon problems and stubborn soft tissue pain. A simple way to explain it is that it can help "wake up" an area where healing and remodeling have stalled.
Patients often ask what it feels like. The answer depends on the body part and irritability level, but most describe it as strong, focused pulses rather than a passive spa-style treatment. It should be part of a broader plan, not a standalone miracle.
Dry needling or acupuncture-based care
Needling approaches can be useful when trigger points, protective muscle tone, or persistent pain are keeping movement from normalizing. They don't replace loading and retraining, but they can reduce the resistance your body puts up when tissues stay guarded.
For people comparing recovery modalities more broadly, this overview of the Benefits of red light therapy for tendons is a useful companion read because it helps frame where light-based recovery tools may fit alongside exercise and hands-on care.
Here is a visual example of movement-focused rehab in action:
What works and what usually doesn't
The best treatment plans combine methods with a clear purpose. They don't just collect techniques.
What usually works well
- Targeted exercise: Because it rebuilds tolerance and control.
- Hands-on treatment with a reason: When it supports better movement afterward.
- Progression: When the program changes as your body changes.
- Specificity: When rehab matches the actual demands of your sport.
What tends to disappoint
- Passive care only: Relief without retraining rarely lasts.
- Generic handouts: The body adapts to precision, not to randomness.
- Returning based on pain alone: Feeling better and being ready aren't the same thing.
One practical option in Deerfield Beach is MedAmerica Rehab Center, which offers physical therapy, hands-on care, acupuncture, and shockwave therapy as part of individualized treatment plans. The important point isn't the menu of services by itself. It's whether each tool is matched to your movement problem and recovery stage.
Building Resilience and Preventing Future Injuries
A successful rehab plan is a partnership. The clinic gives direction, progression, and feedback. The patient supplies consistency.
That matters because tissues don't adapt from one excellent appointment. They adapt from repeated, appropriate loading over time. That's why the home program is not homework in the annoying sense. It's the bridge between what happens in treatment and what your body can do out in the world.
Your role is bigger than most people think
People usually improve fastest when they stop looking for one perfect session and start respecting the cumulative effect of steady work.
That often means:
- Doing the prescribed exercises consistently: Not just when pain spikes.
- Modifying training appropriately: Backing off enough to heal, but not disappearing from movement.
- Watching response patterns: Morning stiffness, next-day soreness, and confidence under load all matter.
- Sleeping, hydrating, and eating well enough to recover: Basic, but often overlooked.
If your training volume is high, nutrition becomes part of recovery too. This article on the impact of exercise on supplement needs is a useful read for active adults trying to match recovery demands with what their body needs.
Recovery is rarely linear. A harder day doesn't always mean damage. It often means your plan needs adjustment, not abandonment.
Prehab is easier than rehab
Many injuries are more preventable than people realize. Neuromuscular injury prevention programs that focus on proprioception, balance, and strength have been shown to reduce injury risk by 37 to 47 percent according to injury prevention guidance in sport.
That doesn't mean every injury can be avoided. Sport carries real risk. But it does mean many athletes can improve their odds with the right habits before pain starts.

What prehabilitation looks like in real life
Prehab doesn't need to be fancy. It needs to be repeatable.
A practical injury-resilience routine often includes:
- Balance work: Single-leg stance, reach drills, controlled instability
- Strength work: Hips, calves, trunk, shoulder support muscles
- Landing and deceleration practice: Teaching the body how to absorb force
- Mobility where it's limited: Not random stretching everywhere
- Load planning: Building training volume without sharp jumps
This matters for more than elite athletes. Many people in community sports don't have regular access to a full sports medicine team. That makes simple, low-barrier prevention strategies even more important. A few focused exercises done well and done regularly can protect a lot of training time.
Durability is built, not granted
The athletes who stay active longest aren't always the most talented. Often, they're the ones who listen earlier, train smarter, and treat recurring warning signs as useful information.
If your last injury taught you anything, let it be this. Don't aim to return as the same version of yourself that got hurt. Return with better strength, better control, and a better system.
Start Your Recovery in Deerfield Beach Today
If you're tired of chasing symptoms, the next step is simple. Get the injury assessed in a way that looks at the whole movement pattern, not just the painful body part.
That approach matters whether you're dealing with a fresh sprain, a stubborn tendon problem, post-surgical weakness, or a recurring ache that's been interrupting training for months. The right plan should identify the source of overload, match treatment to the stage of healing, and give you a clear path back to activity.
For local patients, physical therapy in Deerfield Beach can include the same core elements described throughout this guide: hands-on manual therapy, progressive exercise, biomechanical thinking, and advanced options such as shockwave therapy when appropriate. Since 1995, MedAmerica Rehab Center has served the community with a multidisciplinary model and a patient-centered environment that fits both active adults and more complex rehab cases.
You don't need to wait until the problem becomes severe. If an injury keeps returning, changes how you move, or stops you from doing the activities you enjoy, that's enough reason to act.
The sooner the cause is identified, the sooner recovery starts making sense.
Frequently Asked Questions About Sports Physiotherapy
Practical questions often stop people from booking care even when they know they need it. Here are straightforward answers.
FAQs
| Question | Answer |
|---|---|
| Do I need to be an athlete to benefit from sports injury physiotherapy? | No. It helps anyone whose pain is tied to exercise, recreation, lifting, running, court sports, golf, gym training, or other active movement. |
| What should I wear to the first appointment? | Wear comfortable clothing that lets the therapist see and test the injured area. Athletic shorts, a T-shirt, and supportive shoes usually work well. |
| Will treatment hurt? | Some testing or exercise may reproduce mild symptoms, but treatment should be purposeful and tolerable. Rehab should challenge you without feeling reckless. |
| How many visits will I need? | That depends on the injury, irritability, goals, and how consistently you follow the plan at home. A good clinician should give you a clear working plan, then adjust based on response. |
| Can I keep training while in rehab? | Often yes, but with modifications. Many people do better when training is adjusted rather than stopped completely. |
| What if I've already tried rest, ice, and stretching? | That usually means it's time for a deeper assessment of strength, control, and biomechanics rather than more guesswork. |
If you're ready for a clearer plan and a more complete recovery, contact MedAmerica Rehab Center. The clinic offers patient-centered care for sports injuries, post-surgical rehab, pain relief, and movement restoration in Deerfield Beach.

