Symptoms of Degenerative Discs in Neck: Find Relief
You wake up, turn your head toward the alarm, and feel that same pull at the base of your neck again. Not a dramatic injury. Not the kind of pain that drops you to the floor. Just that stubborn ache and stiffness that keeps showing up when you drive, work at a computer, look down at your phone, or sit too long.
A lot of people in Deerfield Beach live with that pattern for months before they get answers. They assume it’s “just stress,” “bad posture,” or a kink that should’ve gone away by now. Sometimes it is a temporary strain. But when the discomfort keeps returning, spreads into the shoulder or arm, or starts limiting how far you can turn your head, there may be more going on inside the neck.
One common reason is cervical degenerative disc disease, often shortened to cervical DDD. The name sounds harsher than the condition usually behaves. In plain English, it means the discs in your neck have started to wear down over time. That can be irritating, painful, and frustrating, but it’s also something we deal with every day in conservative care.
The good news is that the symptoms of degenerative discs in neck usually make sense once you understand the mechanics. And when the mechanics make sense, treatment becomes much less intimidating. The right plan often includes movement, hands-on care, posture work, and simple home strategies, not panic.
If your neck feels chronically tight, your shoulders seem to carry all your tension, or your arm symptoms are making you wonder what’s normal, start by learning what your body may be telling you. Good daily habits help too, especially if your posture has been drifting over time. These easy exercises you can do at home to improve your posture are a practical place to begin.
That Persistent Ache in Your Neck Might Be More Than a Kink
A temporary neck cramp usually has a clear story. You slept awkwardly. You lifted something poorly. You spent a weekend painting a ceiling. It hurts, then settles down.
Degenerative disc irritation behaves differently. It tends to linger in the background and then flare. One week it feels like stiffness and pressure. Another week it turns into sharper pain after a long drive or a full day at the desk.
That pattern matters.
Many people describe it as a “deep ache” or a feeling that the neck just isn’t moving the way it used to. They rub the muscles, stretch hard, maybe hear a few pops, and get a little relief, but it never fully goes away. Over time, the surrounding muscles start guarding the area, which can make the whole upper trapezius and shoulder blade region feel tight too.
Practical rule: If your neck pain keeps repeating the same cycle of stiffness, flare-up, temporary relief, and return, treat it like a mechanical issue that deserves a proper evaluation.
The term degenerative disc disease often scares people because it sounds like something aggressive. In practice, it usually reflects gradual wear in the discs that sit between the vertebrae. Those discs don’t fail all at once. They change over time, and your symptoms often change with them.
That’s why this problem is manageable. The body can calm irritated tissues, improve support around the neck, and reduce pressure on sensitive joints and nerves. But the plan has to fit the problem. Random stretching, constant cracking, or waiting it out for another six months usually isn’t enough.
What Is Happening Inside Your Neck
Your neck is built to balance mobility with support. Seven cervical vertebrae stack like small building blocks, and a disc sits between most of them to absorb pressure and help each segment move with control.
A healthy cervical disc works like a shock absorber and spacer at the same time. It holds water, gives the neck some spring, and helps nearby bones glide without too much friction or compression.
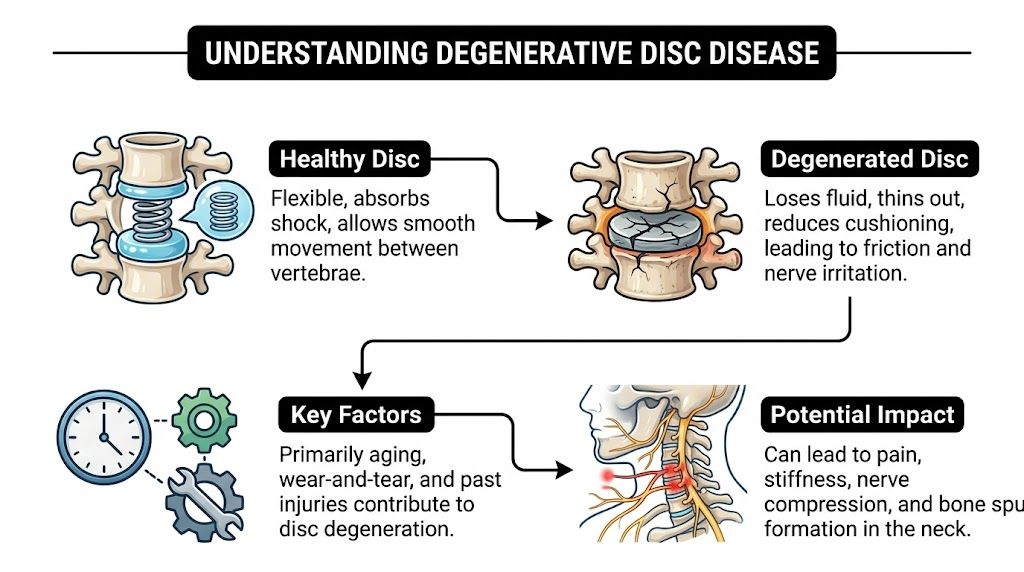
Discs lose hydration and height
With age, repetitive loading, past injuries, and long periods of poor neck mechanics, discs can lose water content and become thinner. That change reduces their ability to cushion force. The result is a neck segment that handles movement less comfortably and less efficiently.
This process often develops slowly. Patients rarely feel one exact moment when a disc "went bad." More often, the disc becomes less resilient over time, and nearby structures start picking up stress they were not designed to handle all day.
That extra stress can affect more than the disc itself. The small facet joints in the back of the neck may get irritated. Supporting muscles may tighten to protect the area. If the space around a nerve narrows, nerve tissue can become sensitive too.
Why one irritated level affects the whole system
The cervical spine works as a chain. If one level stops moving well or loses some of its normal cushion, the levels above and below often compensate. That is why a disc problem can create more than one type of symptom and why treatment needs to address the whole region, not just the sore spot.
In the clinic, I often explain it like this. If one link in a moving chain gets stiff, the surrounding links start doing extra work. In the neck, that means muscles guard, joints compress, and everyday movements such as turning the head, looking down, or holding posture at a desk become harder than they should be.
| Part of the neck | Healthy function | What degeneration changes |
|---|---|---|
| Disc | Cushions and distributes load | Loses water, height, and shock absorption |
| Facet joints | Guide and limit motion | May take on extra stress and become irritated |
| Muscles | Support posture and movement | Often tighten and fatigue as they protect the area |
| Nerves nearby | Carry signals to the shoulder, arm, and hand | Can become irritated if available space decreases |
The source of pain is not always one structure. A degenerated disc can set off a mechanical chain reaction.
That is also why good conservative care usually works best as a coordinated plan. Physical therapy can improve mobility, posture, and strength. Chiropractic care may help restore joint motion where it is restricted. Acupuncture can reduce pain and calm muscle guarding. Used together, these approaches often help patients in Deerfield Beach reduce flare-ups and move with more confidence, without jumping straight to surgery.
None of this means your neck is fragile. It means the area needs better support, better movement patterns, and a treatment plan that matches what is happening inside the joint system.
How Degenerative Disc Disease Makes Itself Known
The symptoms of degenerative discs in neck usually don’t arrive as one clean, obvious sign. They tend to show up in clusters. Some people mainly feel pain and stiffness in the neck itself. Others feel symptoms traveling into the shoulder blade, arm, or hand.

Local neck pain and stiffness
This is the most common starting point. The pain may feel dull, sore, or achy. Some patients say the neck feels “compressed.” Others describe a constant need to stretch.
Stiffness is often worse after being still. You sit through a movie, work at the computer, or wake up in the morning and feel like your head doesn’t want to turn naturally. The first few movements can be the hardest.
Flare-ups are common too. A person may do fairly well for days, then have a rough stretch that lasts hours, days, or longer. That stop-and-start pattern is one reason people underestimate the problem at first.
Pain that travels into the shoulder or arm
When a disc or nearby changes irritate a nerve root, symptoms can move beyond the neck. This is often what people mean by a “pinched nerve.”
Instead of a local ache, the pain can shoot, burn, or feel electric as it travels into the shoulder, down the arm, or toward the hand. It’s often on one side.
Spine-health notes that radiculopathy, meaning radiating arm pain, weakness, or sensory changes, is reported in 15 to 25% of symptomatic patients, and symptoms often worsen with prolonged sitting, which can increase disc pressure by 30 to 40% (Spine-health on cervical degenerative disc disease symptoms and diagnosis).
That’s why desk work can be such a trigger. Sitting isn’t always restful for the neck. If your head drifts forward and your shoulders round, irritated tissues stay loaded.
Numbness, tingling, and odd sensations
Pain isn’t the only nerve symptom. Some people feel pins and needles, tingling in the fingers, or patches of numbness. Others say the arm feels “asleep” or “different,” even when they can’t describe it clearly.
These sensory changes matter because they help tell us that the issue may involve more than tight muscles. They can also help identify which nerve is irritated based on where the symptoms travel.
Nerve symptoms usually follow a path. Muscle tension is more diffuse. That difference helps guide treatment.
A useful example is the person who feels pain near the lower neck and shoulder blade, then tingling into the thumb or fingers after typing, driving, or sitting on the couch looking down. That pattern often points to nerve irritation rather than a simple strain.
Here’s a short visual overview if you learn better by seeing movement and anatomy:
Weakness and loss of function
Weakness is the symptom people often miss until it affects a task. You may not think “my arm is weak.” You may just notice that lifting a pan, carrying a bag, reaching overhead, or gripping a bottle cap feels less steady.
When the neck is involved, weakness can show up as:
- Grip changes: opening jars, carrying grocery bags, or holding tools feels harder.
- Arm fatigue: the shoulder or upper arm gives out sooner than usual.
- Fine motor trouble: buttons, zippers, or typing may feel clumsier.
- Protective avoidance: you stop using one arm normally because it provokes symptoms.
That doesn’t always mean severe damage. It does mean the problem deserves a closer look.
Headaches and upper shoulder tension
Some people with cervical disc degeneration also develop headaches, often near the base of the skull. These can feel different from a migraine. More pressure, more tension, less throbbing.
The upper trapezius, levator scapulae, and other support muscles often tighten as they try to protect a neck that isn’t moving well. Patients then focus on the tight muscles, which is understandable, but those muscles are often reacting to the underlying joint and disc mechanics.
That’s an important trade-off in treatment. Massage alone may feel good, but if no one addresses joint mobility, posture, nerve irritation, and muscle control, relief often fades quickly.
Recognizing Red Flags and When to See a Doctor
A common Deerfield Beach scenario goes like this. Your neck has bothered you for weeks, then one morning you notice you are fumbling your keys, dropping a coffee mug, or feeling unsteady when you turn quickly. That is the point where neck pain stops being a simple soreness problem and needs a closer medical look.
Many cases of cervical disc degeneration respond well to conservative care. The concern changes when the irritated disc and nearby joints start affecting a nerve root or, more seriously, the spinal cord. The spinal cord works like the main cable line for movement, balance, and coordination. Pressure there can change more than pain.
Common symptoms versus urgent concerns
Use this table as a practical guide, not a substitute for an exam.
| Symptom | What It Typically Means | Recommended Action |
|---|---|---|
| Mild to moderate neck ache | Mechanical irritation, disc or joint stiffness, muscle guarding | Schedule a non-urgent evaluation with a clinician |
| Pain into one shoulder or arm | Possible nerve root irritation | Get assessed soon, especially if it keeps returning |
| Tingling or numbness in the hand | Sensory nerve involvement may be present | Seek medical evaluation if it persists or worsens |
| Noticeable arm weakness | Nerve compression may be affecting muscle function | See a doctor promptly |
| Trouble with balance or coordination | Possible spinal cord involvement | Seek urgent medical assessment |
| Changes in bowel or bladder function | Can be a serious neurologic warning sign | Seek immediate medical care |
| Rapidly worsening symptoms | Escalating nerve or cord irritation | Do not wait. Get urgent evaluation |
Signs that should raise concern
Pain, stiffness, and intermittent arm symptoms often allow time for a scheduled evaluation. Loss of hand coordination, repeated falls, clear weakness, or bowel and bladder changes do not.
In the clinic, I tell patients to pay attention to function. Can you button a shirt normally? Type at your usual speed? Carry a bag without your hand giving way? Those details matter because neurologic problems often show up in daily tasks before people describe them as "severe pain."
Safety point: Spreading pain matters. Progressive weakness, clumsiness, or balance changes matter more.
What a doctor or rehab provider may check
A good exam looks at more than where it hurts. Your provider may check reflexes, strength, sensation, walking balance, hand coordination, and which neck positions reproduce or ease symptoms. That helps sort out a mechanical neck problem from a nerve issue and from possible spinal cord involvement.
Imaging is not automatic. It becomes more useful when symptoms are persistent, worsening, or clearly neurologic. If you want a clearer sense of which test fits which situation, this guide on when do you need an MRI and when do you need an X-ray explains it in plain language.
Sleep setup also matters more than many people realize. A poor pillow setup can keep the neck slightly twisted for hours and leave already sensitive tissues irritated by morning. If nighttime positioning is part of your pattern, this guide on choosing the right bed support pillows is a useful starting point.
The good news is that red flags are not the whole story. Many patients need timely evaluation, not surgery. In our setting, that often means coordinating physical therapy, chiropractic care, acupuncture, and medical follow-up so the right problem gets treated at the right pace.
Finding Relief Without Surgery
The best non-surgical care doesn’t chase symptoms blindly. It identifies what’s driving them.
If your neck is stiff because joints aren’t moving well, you need mobility work. If irritated nerves flare when you sit, you need posture correction and load management. If muscles are guarding because the neck lacks support, you need strength and control, not endless stretching.
Physical therapy addresses the mechanics
Physical therapy is often the backbone of treatment because it improves how the neck functions under real-life demands. That means restoring motion where motion is limited, improving muscle support where stability is lacking, and teaching positions that reduce repeated irritation.
According to Top Orthopedics, targeted physical therapy emphasizing McKenzie extension exercises and isometric stabilization can reduce pain by 50% in 6 to 8 weeks by restoring the neck’s natural curve and reducing disc pressure (Top Orthopedics on degenerative disc disease in the neck).
That matters because random exercise isn’t the same as targeted exercise. The right movement tends to calm symptoms. The wrong movement, done too often, can keep feeding them.

Chiropractic care can help restore motion
When the neck and upper back get restricted, patients often feel stuck in the same painful pattern. Careful joint mobilization or manipulation may help improve motion in segments that aren’t moving well.
The trade-off is that this works best when it’s part of a larger plan. A quick adjustment may create temporary relief, but if sitting posture, muscle endurance, and daily mechanics don’t improve, symptoms can return fast. Manual treatment opens a window. Exercise helps you keep it.
Acupuncture can calm an irritated system
Acupuncture is useful for some patients who are dealing with persistent pain, protective muscle tension, or flare-sensitive symptoms. It doesn’t “put the disc back,” and it shouldn’t be sold that way. What it can do is help reduce pain sensitivity and make it easier to tolerate movement-based rehab.
That combination matters. When pain settles enough for you to move normally again, you can strengthen the system that supports recovery.
Home care needs to be simple enough to repeat
Most successful plans include a short home routine. Not a complicated workbook. Just a few focused habits done consistently.
Examples include:
- Posture resets: gentle chin tuck positioning, shoulder blade setting, and frequent changes in sitting posture.
- Movement breaks: standing up regularly if desk time triggers symptoms.
- Heat or ice: based on which one calms your symptoms better.
- Sleep support: a pillow that keeps the neck in a neutral position often helps morning stiffness.
For sleep, one useful reference is this guide on choosing the right bed support pillows, especially if you wake with more pain than you had when you went to bed.
The goal at home isn’t to do more. It’s to do the few things that actually reduce irritation.
What usually doesn’t work well
Patients often lose time on strategies that feel active but don’t change much.
A few examples:
Aggressive self-cracking
It may feel relieving for a moment, but it rarely improves the underlying control problem.Stretching into nerve pain
If tingling increases as you “stretch,” that’s often not a productive stretch.Resting too much
Short-term rest helps during a flare. Too much rest usually increases stiffness.Using one treatment in isolation
Massage alone, acupuncture alone, or exercise alone may help somewhat. Many neck cases improve more clearly with a coordinated plan.
If you want a deeper understanding of physical therapy's role, this guide on how physical therapy helps with back and neck pain – a guide is a valuable resource.
How We Help Patients in Deerfield Beach Get Back to Life
Patients who come in for neck pain aren’t looking for a lecture. They want to know what’s causing the symptoms, whether it’s fixable, and what they should do next.
That first visit usually starts with listening. When did the symptoms begin. What movements trigger them. Is the pain local, or does it travel. Is sleep affected. Are there numbness or weakness symptoms. Those details shape the plan more than any buzzword diagnosis.
Care starts with what your neck is actually doing
A useful exam looks at more than where it hurts. We check how your neck moves, how the upper back contributes, whether certain positions centralize or aggravate symptoms, and how your shoulders and posture interact with the problem.
From there, treatment is customized. One patient may need more manual therapy and mobility work. Another may need nerve calming strategies and gradual strengthening. A third may need a mix of physical therapy, chiropractic care, and acupuncture because the pain has become persistent and layered.
That coordinated approach is especially helpful for adults trying to stay active while managing work, driving, family responsibilities, or recovery after an auto accident. You don’t need ten different opinions. You need one clear plan that fits your symptoms and your day.
The end goal is function
Less pain matters. But function matters more.
We want you turning your head while driving without bracing. Sleeping without waking up stiff. Working at your desk with fewer flare-ups. Carrying groceries, walking the beach, exercising, and getting through an ordinary week without your neck controlling the schedule.

When patients understand the symptoms of degenerative discs in neck, they usually feel less anxious and more ready to act. That shift matters. The condition may be common, but your treatment still needs to be personal, practical, and consistent.
If neck pain, arm symptoms, or recurring stiffness are starting to limit your day, MedAmerica Rehab Center offers conservative care that can help you understand the cause, reduce irritation, and build a realistic recovery plan. A focused evaluation can show whether physical therapy, chiropractic care, acupuncture, or a combination makes the most sense for your specific symptoms.

