How to Treat a Pulled Muscle in Leg: A Complete Guide
You’re moving normally, then it happens. A quick sprint, a missed step, a heavy lift, or even getting up awkwardly, and suddenly there’s a sharp pain in your leg. Sometimes it feels like a grab. Sometimes it feels like a snap or a cramp that won’t let go. In that moment, a common question arises: Did I just pull a muscle, and what do I do now?
A pulled muscle in the leg is usually a muscle strain, which means some of the muscle fibers have been overstretched or torn. Mild strains can feel sore and tight but still let you walk. More involved strains can cause limping, swelling, weakness, or bruising. Severe strains can make it hard to use the leg at all.
Most leg strains, especially Grade I and Grade II injuries, heal with conservative care rather than surgery, according to Mayo Clinic’s muscle strain guidance. The part many people miss is that recovery isn’t just about icing and waiting. Early first aid matters, but so does the shift from protection to controlled movement. That transition often determines whether the muscle heals cleanly or stays stiff, weak, and easy to re-injure.
That Sudden Pain in Your Leg What to Do First
A classic strain story sounds familiar. You’re jogging, cutting sideways on a court, climbing stairs with groceries, or lifting something heavier than expected. You feel a sudden pull in the calf, hamstring, quad, or groin. The leg tightens immediately. You try to “walk it off,” and the pain argues back.
That first reaction matters. If the pain came on suddenly during effort, assume the muscle needs protection right away. Don’t stretch aggressively. Don’t test it by repeating the movement. Don’t keep training to see if it loosens up.
How severe does it seem
A simple way to think about a leg strain is by how much function you still have.
- Mild strain means the leg is sore and tender, but you can still move it and put weight on it.
- Moderate strain usually brings a more noticeable limp, tighter movement, swelling, and weakness.
- Severe strain may feel dramatic from the start. You may hear or feel a pop, lose strength, or find it very hard to walk.
Practical rule: If pain changes the way you walk, the injury is more than “just tightness.”
The first decision to make
Your job in the first stretch of recovery is simple. Calm the area down and avoid making the tear bigger. That means reducing bleeding into the muscle, controlling swelling, and not loading tissue that’s just been injured.
People often go wrong in one of two ways. They either do too much too soon because they’re worried about losing fitness, or they do too little for too long and let the muscle stiffen up. If you want a clear answer to how to treat a pulled muscle in leg, the best plan is phased. Start with protection, then add movement, then rebuild strength carefully.
Your First 48 Hours The RICE Protocol Explained
The first 48 hours set the tone for the rest of recovery. The goal is simple. Protect the torn fibers, limit extra bleeding into the muscle, and keep swelling from getting ahead of you. That is where RICE still earns its place: Rest, Ice, Compression, and Elevation.
RICE is useful, but it is not the whole treatment plan. In clinic, I treat it as the acute-phase tool kit, not the finish line. It helps calm things down early so you can make a cleaner shift into gentle movement and strengthening instead of dragging the injury out and building more stiffness than necessary.

What each step is doing
Rest means relative rest. You are protecting the muscle from movements that increase the tear, not putting yourself on complete shutdown. If walking causes a limp, shorten your trips, slow down, and reduce load. A more painful hamstring or groin strain may need temporary support such as crutches.
Ice is mainly for pain control and limiting early swelling. Use a towel between the pack and your skin, and keep each session brief. For a fresh strain, an ice pack is usually the practical choice. If you want a comparison of cold methods, you can discover ice bath duration, but long cold exposure is not the goal here.
Compression gives the area light support and helps manage swelling. An elastic wrap should feel snug, not tight. If your foot starts tingling, throbbing, getting cold, or changing color, loosen it.
Elevation helps fluid drain instead of pooling in the injured leg. Prop the leg up when you are resting, especially if swelling is obvious by the end of the day.
For practical guidance on timing and skin safety, this overview of using an ice pack in physical therapy is a useful reference.
First 48 Hours Care Do's and Don'ts
| Action | What to Do (The 'Do's') | What to Avoid (The 'Don'ts') |
|---|---|---|
| Rest | Reduce activity and protect the leg from painful loading | Playing through pain or testing it with explosive movement |
| Ice | Apply for short sessions every few hours during the early phase | Leaving ice on continuously or placing it directly on bare skin |
| Compression | Use an elastic wrap that feels supportive but not restrictive | Wrapping so tightly that the leg tingles, throbs, or changes color |
| Elevation | Raise the leg during rest to help manage swelling | Letting the leg stay down for long periods when it’s already swelling |
| Activity | Move only within a comfortable range for essential daily tasks | Deep stretching, massage guns, hard workouts, or “pushing through” |
A short movement demo can also help you understand how clinicians think about early strain care:
More ice is not better. Correct timing is better.
A real trade-off with RICE is that it is widely used in practice, but it has not been definitively proven in randomized clinical trials, as noted earlier from Mayo Clinic. That does not make it useless. It means you should use it for what it does well: early symptom control and protection. Then, once the leg is less reactive, shift into the active part of recovery instead of staying stuck in rest mode for too long.
Managing Pain and Beginning Gentle Movement
Around day 2 or 3, the job changes. The muscle still needs protection, but too much rest now can leave it stiff, guarded, and slower to recover. This is the point where many leg strains either start progressing well or get stuck.
Pain control should support movement, not just numb symptoms. Some clinicians use NSAIDs such as ibuprofen or naproxen after a muscle strain, while others prefer to avoid them in the first couple of days because of bleeding concerns and use acetaminophen instead. If you have a history of stomach ulcers, kidney disease, blood thinners, or medication interactions, check with your physician or pharmacist before taking anything.
Heat can make sense once the leg no longer feels hot and actively swollen. I usually tell patients to match the tool to the problem. Ice is for an irritated, reactive muscle. Gentle warmth is often better for a muscle that feels tight, guarded, and hard to get moving before a short walk or light exercise.
This stage matters because muscle tissue heals better with the right amount of motion. Too little movement and the area stiffens. Too much load too soon and the strain gets stirred up again. The goal is calm, repeatable motion that tells the healing tissue how to line up without asking it to produce force it cannot handle yet.
Start with simple movement for a few minutes at a time:
- Ankle pumps or circles if you have been limping or sitting more than usual
- Heel slides on the bed or floor to restore easy leg motion
- Slow knee bends without weight if they stay comfortable
- Short, even-paced walks only if you can avoid a noticeable limp
Good early movement is boring on purpose. That usually means you are in the right zone.
What should it feel like? Mild pulling, light effort, and a little stiffness at the start are all common. Sharp pain, a sudden grab, cramping, or limping that gets worse means the load is too high. Back off, rest, and try a smaller range or shorter session later that day.
If the leg is settling down, this is also a reasonable time to begin very basic muscle activation and then build toward strength. A simple progression with leg-strengthening exercises for recovery and support can help once pain is under control and daily walking is getting easier.
Nutrition comes up a lot here. Keep expectations realistic. Supplements do not replace graded rehab, but some people like to review the options. VitzAi.com's recovery advice is a reasonable starting point for general reading. The bigger driver of recovery is still how well you manage load, motion, and the return to strength.
Your Recovery Timeline and At-Home Exercises
A pulled muscle usually feels much better before it is ready for full activity. That gap is where re-injury happens.
The first part of recovery is about calming the tissue down. The next part is where you start to shape how that muscle heals. If you rest too long, the leg gets stiff, weak, and less tolerant of load. If you push too soon, the healing fibers get irritated and you can end up back at the start. Good rehab is the middle path. Protect the muscle early, then add movement and strength in a steady way so scar tissue stays more flexible and the leg can handle real life again.
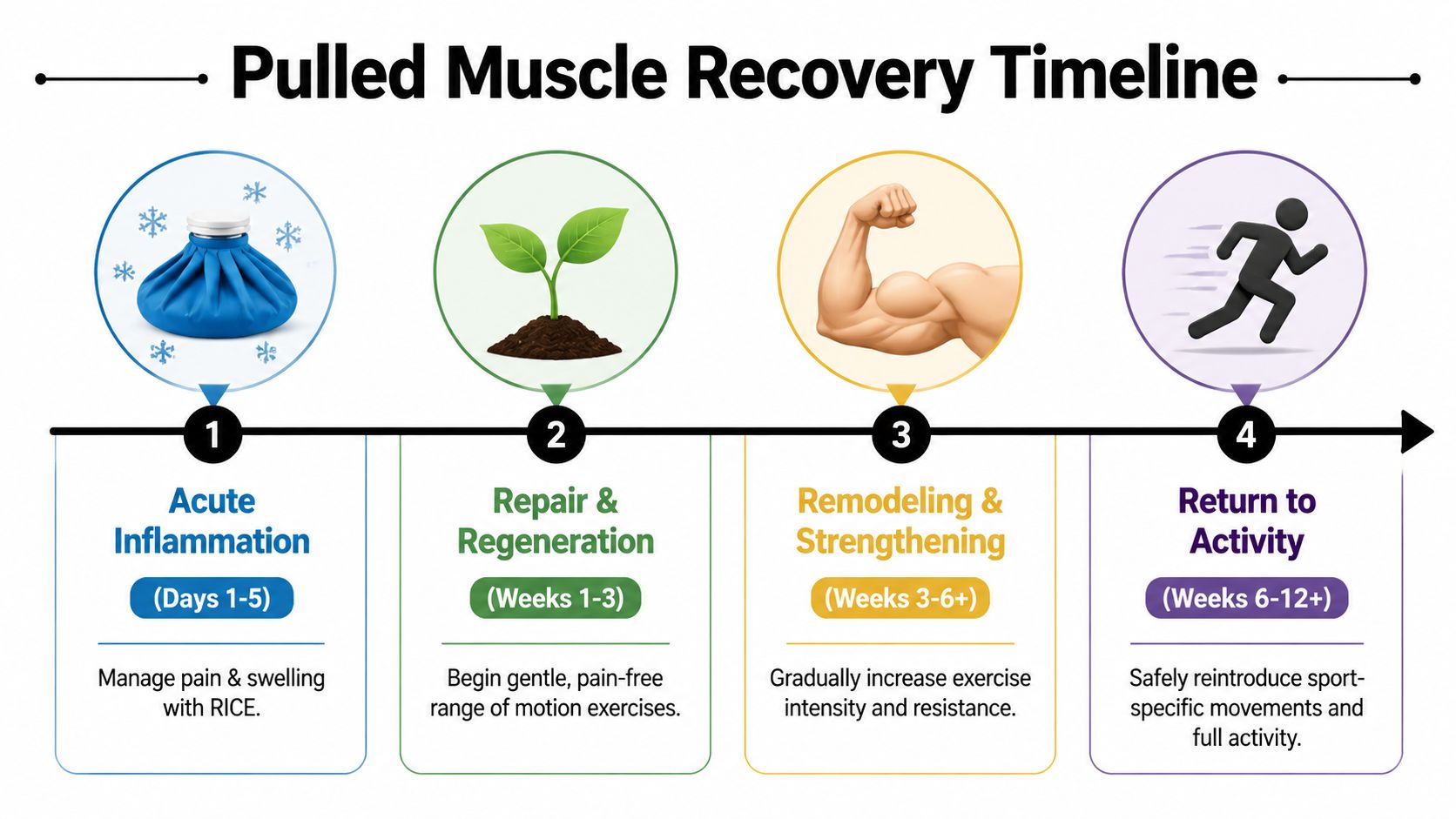
Why the timeline matters
I tell patients to use milestones, not the calendar alone. Two people can have the same diagnosis and recover at different speeds based on the size of the strain, the muscle involved, age, training history, and how much they irritated it in the first week.
A simple home progression looks like this: first get walking more normally, then restore easy muscle contraction, then add light stretching and bodyweight strength, and only after that return to hills, sprinting, jumping, or sport. The goal is not just less pain. The goal is a muscle that can contract, lengthen, and absorb force without guarding.
Safe at-home exercises to start with
Start these once sharp pain has settled and the leg does not feel worse a few hours later or the next morning. Mild pulling is acceptable. Sharp pain, cramping, or a more obvious limp means the exercise is too aggressive right now.
Hamstring set
Lie on your back with the knee slightly bent. Press your heel gently into the floor or bed without moving the leg. Hold briefly, then relax. Start with easy effort, not a max squeeze.Quad set
Sit or lie with the leg straight. Tighten the front of your thigh and press the knee down gently. This works well when the leg still feels hesitant with bending or straightening.Calf isometric
Sit with the foot on the floor and press the ball of the foot down lightly, as if beginning a calf raise without lifting the heel. This is a good first step after a mild calf strain.Seated hamstring stretch
Straighten the knee only until you feel light tension. Stay out of pain and skip bouncing. Early stretching should restore motion, not force it.Standing weight shift
Hold a counter and shift weight side to side. This helps the injured leg accept load again and often exposes whether walking mechanics are improving.
Once those feel easy and your walking is smoother, add more deliberate strengthening. These leg-strengthening exercises for recovery and support are a reasonable next step.
A realistic progression
Use these checkpoints to decide if you are ready for more:
- You can walk without a clear limp
- You can tighten the injured muscle without a pain spike
- You can tolerate a light stretch without guarding
- You can handle bodyweight loading before adding speed or impact
That sequence matters. A calf strain that feels fine during daily activity can still fail during push-off. A hamstring can feel loose enough to stretch but still be too weak to handle a quick step or jog. Pain going down is only part of recovery. Strength and load tolerance have to catch up.
Some athletes also read about broader recovery options, including a peptide for athletic recovery. Keep expectations grounded. No supplement or peptide replaces graded loading, consistent exercise, and good timing.
When to See a Physical Therapist at MedAmerica Rehab
A lot of leg strains calm down with home care, then stall. Pain starts to fade, but the muscle still feels weak, tight, or unreliable when you try to walk faster, climb stairs, or get back to exercise. That is usually the point where an exam helps, because recovery is no longer just about protecting the area. It is about restoring motion, strength, and timing so the muscle can handle load again without flaring up.
A physical therapy visit is a smart next step if you felt a pop when the injury happened, cannot bear weight normally, have obvious bruising or swelling, or keep limping after the first few days. Repeated setbacks matter too. If the same spot grabs every time activity picks up, the tissue may be healing, but not in a way that tolerates real-life demands.

What a clinic can do that home care can’t
The biggest difference is progression. At home, many people rest until it hurts less, try a stretch, then jump back into normal activity. In the clinic, we test what the muscle can do. That includes checking range of motion, pain with contraction, strength at different angles, balance, gait, and how the leg responds to loading.
Treatment may include hands-on work to improve mobility, guided exercise to rebuild strength without overloading healing tissue, and modalities such as TENS or NMES when they fit the stage of recovery. The goal is not to chase pain alone. The goal is to help the muscle heal with better movement quality, less protective guarding, and less risk of stiff scar tissue limiting the next phase.
That matters more than many people expect. A calf can feel fine during regular walking but still fail during push-off. A hamstring can tolerate a basic stretch and still not be ready for a quick stride, hill, or sprint. Those are the gaps that often lead to re-injury.
At MedAmerica Rehab Center, care for a leg strain may include hands-on treatment, a graded strengthening plan, and clear return-to-activity benchmarks based on how your leg performs, not just how it feels that day. If you have never been to PT before, it helps to see what a typical physical therapy session looks like, because good rehab is a series of well-timed progressions, not a generic sheet of exercises.
If the muscle keeps tightening, catching, or losing strength when you return to normal activity, get it checked. Early guidance often shortens the recovery cycle and helps prevent the same strain from coming back.
How to Prevent a Pulled Muscle in the Future
Most leg strains don’t happen because one muscle is “bad.” They happen because load outruns preparation. A tight hamstring, weak glute, deconditioned calf, poor warm-up, or sudden jump in activity can all feed the same problem.

Habits that lower your risk
Warm up with movement
Start with dynamic motion before exercise. Leg swings, marching, bodyweight squats, and easy lunges prepare tissue better than jumping into full speed cold.Build strength through full range
Muscles tolerate force better when they’re trained gradually and consistently. Don’t only train the front of the legs. Include glutes, hamstrings, calves, and core.Keep flexibility practical
You don’t need extreme stretching. You do need enough mobility to move well without compensating.Respect fatigue
Many strains happen when form gets sloppy late in a workout, game, or long workday.
What people often get wrong
A lot of active adults focus on one prevention tool and ignore the rest. They stretch but don’t strengthen. They train hard but skip warm-ups. They return to sprinting before they’ve rebuilt basic single-leg control. Prevention works better when all the pieces support each other.
Hydration, regular meals, and adequate protein intake help support recovery from training, but they won’t rescue poor loading decisions. The body handles challenge better when sleep, training volume, and recovery are all reasonable.
A good prevention plan usually includes these questions:
- Am I increasing activity too quickly?
- Can I control my leg through the ranges I use?
- Do I still feel uneven side to side after the old injury?
- Am I warming up for the activity I’m about to do, not just doing random stretches?
If you’ve had more than one strain in the same spot, don’t assume it’s just bad luck. Recurrent strains usually point to a strength deficit, motion restriction, or return-to-sport progression that was never fully finished.
If your leg still feels weak, tight, or unreliable after a pulled muscle, MedAmerica Rehab Center can evaluate the strain, guide a stage-appropriate rehab plan, and help you return to walking, work, exercise, and sport with less risk of another setback.

