Living with degenerative disc disease in the neck: Living wi
You wake up, turn your head toward the alarm, and feel that familiar catch in your neck. Later, you sit at your laptop, glance down at your phone, then look over your shoulder while backing out of a parking space. The same stiff, nagging ache shows up again. By evening, it may spread into your shoulder blade or arm and leave you wondering if something serious is happening.
If you have been told you have degenerative disc disease in the neck, the name alone can sound alarming. Many people hear the word “degenerative” and assume their neck will only get worse. That is not how this diagnosis needs to define your life.
Living with degenerative disc disease in the neck is usually about management, movement, and smarter daily habits, not fear. In clinic, I often remind patients that this is a very common age-related change in the cervical spine. What matters most is how your symptoms behave, what makes them flare, and what helps you move with less pain and more confidence.
Your Guide to Navigating Neck Pain and Stiffness
One patient once described her neck pain this way: “It is not always dramatic. It just keeps interrupting my day.” That is how cervical disc problems often feel. Not one major event, but a series of small losses. Less freedom turning your head. More discomfort at the computer. More hesitation when lifting groceries, driving, reading, or sleeping.
You might notice morning stiffness that eases after a hot shower. Or pain that builds after a few hours at a desk. Some people feel a dull pressure at the base of the skull. Others get sharp pain when they rotate their head too quickly.
Those experiences are frustrating, but they are also common. Cervical degenerative disc disease refers to age-related changes in the discs of the neck. It is a manageable condition for many people, and in many cases, the best starting point is conservative care rather than surgery.
Key takeaway: A diagnosis of cervical DDD does not automatically mean severe damage, disability, or an operation. It often means your neck needs better support, better movement, and better daily mechanics.
The goal is not to chase a “perfect” neck. The goal is to help you move more comfortably, work more easily, sleep better, and return to the activities you enjoy. That starts with understanding what is happening inside the neck.
Understanding Cervical Degenerative Disc Disease
The cervical spine is your neck. It is made up of seven vertebrae with discs in between them. Those discs work like cushions. They help absorb force and allow the neck to bend, turn, and support the head through everyday movement.
A simple way to think about discs is to compare them to shock absorbers on a car or the tread on a tire. They are built to handle repeated use. Over time, they can lose some of their water content and flexibility. That natural wear can change how the neck moves and how stress is shared by the joints, muscles, and nerves.
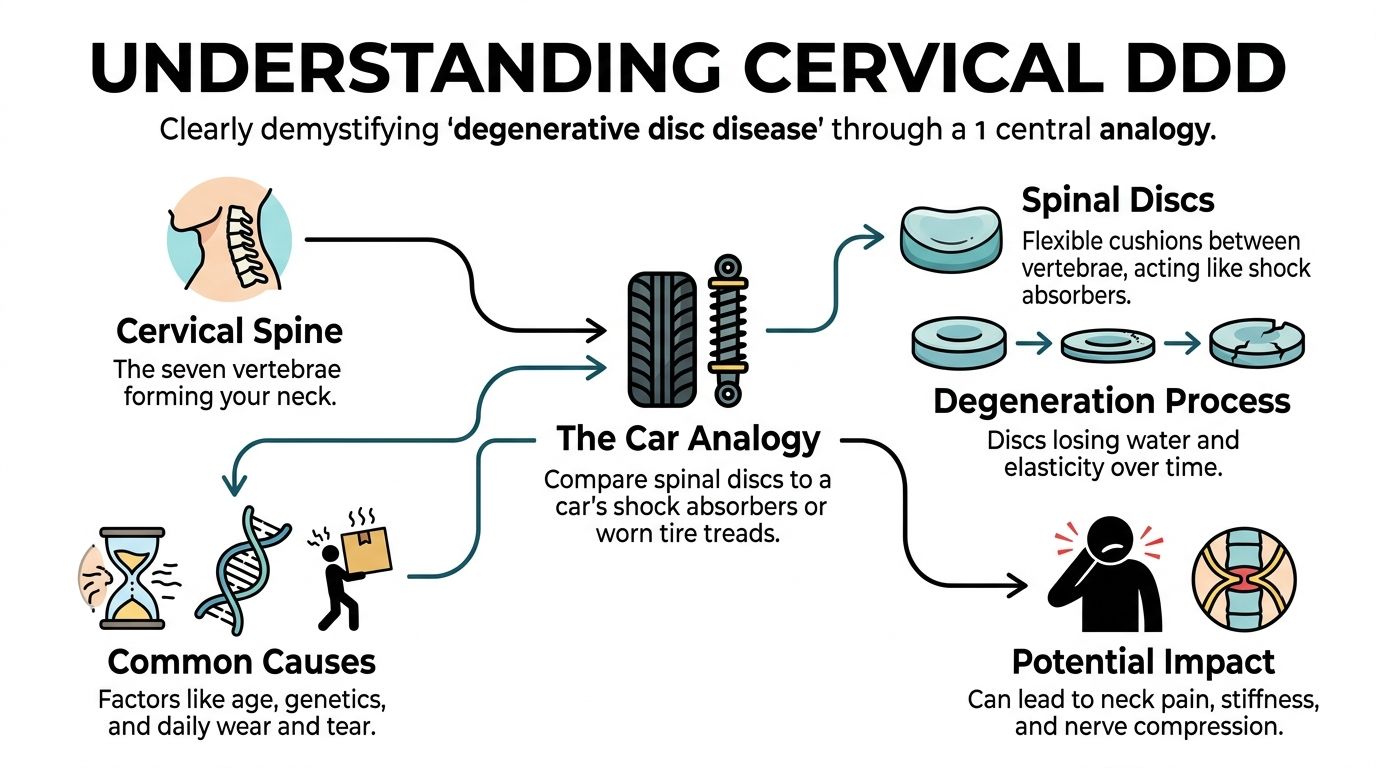
What degeneration really means
The phrase degenerative disc disease is confusing because it is not a disease in the way many people imagine. It usually describes changes that happen with age and use. Genetics, previous strain, posture habits, repetitive movement, and injury history can all influence how early or how strongly those changes show up.
Many people expect an MRI finding to perfectly explain their pain. In reality, imaging and symptoms do not always match. Some people have noticeable disc changes and very little pain. Others have moderate imaging findings and feel quite limited.
That is one reason this diagnosis should be interpreted in context, not in isolation.
How common it is
Cervical disc changes are very common. Disc degeneration is evident in about 25% of individuals under 40, rises to 60% in those age 40 and older, and by age 60 over 90% of people show some evidence on imaging according to the NCBI overview of cervical degenerative disc disease.
The same source notes that the most commonly affected levels are C5-C6 and C6-C7. These are busy segments of the neck. They handle a lot of motion and load, so it makes sense that they often show wear first.
Why this should lower your anxiety
A scan can be helpful, but it can also scare people when they see words like “degeneration,” “bulge,” or “narrowing.” The important point is this: common does not mean catastrophic.
Here is the practical meaning of that idea:
- Aging is part of the picture: Discs change over time just like skin, joints, and eyesight do.
- Imaging is not destiny: A report can show changes without guaranteeing severe pain.
- Symptoms guide treatment: Your pain pattern, strength, motion, and nerve signs matter more than a single scary term on a report.
- The neck responds to care: Muscles, joints, posture habits, and movement patterns can all improve with the right plan.
If your neck has become more sensitive, think of it less as “broken” and more as under-supported and irritated. That shift in thinking helps many people move away from fear and toward action.
Recognizing Symptoms and Getting a Clear Diagnosis
Some people with cervical DDD feel only stiffness. Others notice symptoms that travel. That difference matters.
Pain from the neck can stay local, or it can spread into the shoulder, upper back, or arm. Some people describe burning, tingling, or numbness. Others notice that carrying a bag, working at a desk, or holding the phone to one ear makes symptoms worse.
What symptoms can look like in real life
The common pattern is not just “neck pain.” It may include:
- Local neck pain and stiffness: Often worse after sleeping awkwardly, sitting too long, or staying in one position.
- Radiating pain: Discomfort can move into the shoulder or down the arm.
- Numbness or tingling: This may suggest irritation around a nerve root.
- Muscle weakness: You may feel your grip is less steady or lifting overhead feels harder.
- Headaches: Some people get pain that starts in the neck and refers upward.
- Reduced motion: Turning to check traffic or looking up at a shelf may feel limited.
A published review notes that living with cervical DDD often involves symptoms beyond simple stiffness, including pain radiating to the shoulders or arms, numbness, tingling, and muscle weakness, and that prolonged sitting with poor posture such as tech neck, heavy lifting, and repetitive strain can accelerate progression. The same review reported that males with neck pain had a 90.3% rate of disc narrowing compared with 77.2% in those without pain in one study, while also supporting conservative management for many individuals through the PMC review on cervical disc degeneration and symptoms.
A short visual overview can help if you want to see how these symptoms are commonly explained in patient education.
What happens during an evaluation
A good evaluation usually starts with your story. When did symptoms begin? What movements trigger them? Do symptoms travel? Is sleep affected? Do you feel weakness, clumsiness, or dropping objects?
Then a clinician looks at how your neck and upper back move. They may check:
- Range of motion: Can you turn, bend, and look up without major restriction?
- Strength: Are the shoulder, arm, or hand muscles working evenly?
- Sensation: Do both sides feel the same to light touch?
- Reflexes and nerve tension signs: These help identify whether a nerve may be involved.
- Posture and movement habits: Forward head posture, rounded shoulders, and upper back stiffness often show up here.
When imaging is helpful
Not every person with neck pain needs imaging right away. In many cases, a physical exam gives the most useful information early on. X-rays can show alignment and bony changes. MRI is better when a provider needs to look at discs, nerves, and soft tissue structures.
If you are unsure when each test is useful, this patient guide on when you need an MRI and when you need an X-ray can make that decision process easier to understand.
Tip: The best diagnosis is not just a label. It is an explanation of what structure may be irritated, what movements aggravate it, and what you can start doing about it.
Your Team for Conservative Neck Pain Treatment
When neck pain starts affecting work, driving, sleep, or exercise, many people ask a fair question: “Who should I see first?” The better question is often, “What combination of care will help me move better, feel safer, and calm this down?”
For many individuals living with degenerative disc disease in the neck, the strongest starting point is conservative treatment. That means using non-surgical care to reduce pain, restore mobility, improve strength, and help the neck tolerate daily life again.
Physical therapy and active recovery
Physical therapy is often the foundation. A therapist looks at more than the painful spot. They assess how the neck, shoulder blades, upper back, and even breathing mechanics work together.
A session may include manual techniques, guided exercise, postural retraining, and education on movement habits. The aim is not just temporary relief. It is better support for the neck during normal tasks like typing, lifting, driving, and sleeping.
Patients often do best when therapy focuses on these goals:
- Restoring motion: Gentle movement can reduce guarding and help stiff joints move more freely.
- Building support: Stronger deep neck flexors, upper back muscles, and shoulder stabilizers reduce strain on irritated segments.
- Improving mechanics: Small changes in desk setup, lifting form, and body positioning can lower repeated stress.
- Reducing fear of movement: Many people hold the neck rigidly after pain begins. That stiffness can become part of the problem.
If you want a patient-friendly explanation of this approach, how physical therapy helps with back and neck pain provides a clear overview.
Chiropractic care and joint mobility
Some people with cervical DDD develop stiff joints above or below the irritated level. That can create a cycle where the neck moves poorly, muscles tighten, and pain stays active.
Chiropractic care may help by improving spinal and joint mobility. For the right patient, hands-on treatment can reduce stiffness and improve how the neck and upper back share movement. In practice, this is often most helpful when paired with exercise, not used alone.
The key is matching the technique to the person. Someone with a highly irritable neck may need gentle mobilization rather than aggressive force. A thoughtful clinician adjusts care based on symptoms, age, comfort, and exam findings.
Acupuncture and pain regulation
When pain has been present for a while, the nervous system can become more sensitive. That is one reason some people feel pain from activities that should not hurt as much as they do.
Acupuncture can be useful in a conservative care plan because it may help calm pain, reduce muscle guarding, and make it easier for a person to tolerate movement and exercise. Some patients find it especially helpful when stress, poor sleep, or chronic muscle tension are part of the picture.
It is not magic, and it is not a replacement for strengthening. But it can create a window where the body is less reactive, which makes active rehab easier.
Shockwave therapy and stubborn soft tissue irritation
In some cases, neck pain is not only about the disc itself. Surrounding tissues can become chronically irritated from guarding, altered posture, and repeated overload. That is where a modality like shockwave therapy may be considered as part of a broader plan.
The idea is not that one machine “fixes” cervical DDD. The better view is that certain technologies may help reduce local irritation and support tissue recovery in selected cases, especially when combined with targeted exercise and manual care.
Why combined care often works better
A single treatment style may help, but many people benefit more when care is coordinated. One provider improves pain. Another restores motion. Another builds strength and confidence. Together, those pieces create progress that feels more complete.
Here is how a multidisciplinary plan often works:
| Focus | What it targets | Why it matters |
|—|—|
| Physical therapy | Strength, movement control, posture | Helps the neck tolerate daily demands |
| Chiropractic care | Joint mobility, stiffness | Can improve motion where the neck feels blocked |
| Acupuncture | Pain sensitivity, muscle tension | May help calm flare-ups and improve comfort |
| Shockwave therapy | Persistent soft tissue irritation | Can support recovery in selected cases |
Key takeaway: Conservative care works best when treatment is not passive. The goal is to combine symptom relief with better movement and stronger support.
The best plan is individualized. One person needs help returning to desk work. Another needs to recover after an auto accident. Another wants to garden, sleep through the night, and drive without fear. The diagnosis may be similar. The treatment emphasis should not be identical.
At-Home Pain Management and Lifestyle Adjustments
Clinic visits help, but most of your neck’s day happens at home, in the car, at work, and on devices. That is why daily habits matter so much.
For many people, the biggest hidden trigger is not one dramatic movement. It is hours of repeated forward head posture, especially while using a phone, laptop, or tablet. That pattern is often called tech neck.

A patient education source focused on this issue states that over 60% of adults over 40 report their neck pain has worsened due to increased device use, and emphasizes ergonomic adjustments such as monitor stands and posture breaks in the discussion of things to avoid with degenerative disc disease in the neck.
What tech neck looks like
Tech neck usually shows up in ordinary moments:
- Reading texts with your chin dropped toward your chest
- Working on a laptop that sits too low
- Scrolling in bed with your head propped forward
- Sitting through long meetings without changing position
- Using bifocals in a way that makes you poke your chin out toward the screen
The neck is very good at movement. It is not built to hold the same strained position for long stretches.
Simple changes that reduce flare-ups
You do not need a perfect ergonomic setup to help your neck. You need a setup that reduces repeated stress.
Try these adjustments:
- Raise the screen: Use a monitor stand, stacked books, or an external keyboard so the screen sits closer to eye level.
- Bring the phone up: Lift the phone toward your face instead of bending your head down toward it.
- Use both arms when possible: This reduces asymmetry and shoulder tension during device use.
- Take movement breaks: Stand up, walk, roll the shoulders, and gently reset posture throughout the day.
- Change positions often: The “best” posture is usually the one you do not hold too long.
Heat, ice, and pacing
Heat often helps with muscle tightness and morning stiffness. Ice may feel better during an irritated flare-up, especially after overdoing an activity. Both can be useful. Neither has to be used for long to be helpful.
Pacing matters just as much. If your neck flares every time you clean, cook, or work at the computer for too long, break tasks into smaller blocks. A short pause taken early usually works better than waiting until pain becomes intense.
Sleep and daily activity
Sleep posture can either calm the neck or keep it irritated. Many people do better with a pillow that keeps the neck in a neutral position rather than sharply bent. Stomach sleeping often puts the neck in prolonged rotation, which some people with cervical DDD do not tolerate well.
At home, look for patterns instead of blaming random pain:
- Does reading trigger symptoms?
- Does driving increase tingling?
- Does using a recliner help or worsen your posture?
- Does carrying laundry on one side spike pain later?
Tip: Rest can calm a severe flare, but too much rest often backfires. Gentle movement keeps muscles engaged and helps the neck avoid becoming even stiffer.
Safe Home Exercises and Posture for Neck Health
The neck usually responds better to gentle, consistent exercise than to complete avoidance. The goal is not to stretch aggressively or “crack” the neck into place. The goal is to improve control, mobility, and endurance without provoking symptoms.
Move slowly. Stay in a comfortable range. Mild stretching is fine. Sharp, spreading, or lasting pain is not the target.
Chin tucks for deep neck support
This is one of the most useful starting exercises for people with forward head posture.
- Sit or stand tall.
- Keep your eyes level.
- Gently draw your head straight back, as if making a small double chin.
- Do not tip your head up or down.
- Hold briefly, then relax.
You should feel a gentle engagement deep in the front of the neck, not a hard strain in the throat or jaw. This exercise helps train the muscles that support the head in a more balanced position.
Gentle range of motion work
If the neck has become guarded, easy motion can help restore confidence.
Try these:
- Rotation: Turn your head slowly to one side, then the other.
- Side bending: Bring one ear gently toward the same-side shoulder.
- Looking down and up: Move within a comfortable arc, especially if extension feels limited.
Keep the movement smooth. If one direction feels restricted, avoid forcing it. You are teaching the neck that movement is safe again.
Upper back and chest mobility
A stiff upper back often makes the neck work too hard. Tight chest muscles can also pull the shoulders forward and increase strain.
A simple doorway stretch can help:
- Stand in a doorway.
- Place your forearms on the frame.
- Step through gently until you feel a stretch across the chest.
- Keep the neck relaxed, not poked forward.
You can also practice shoulder blade squeezes. Gently draw the shoulder blades back and down, then release. This supports a more balanced upper body posture.
A simple daily routine
Here is a sample home sequence many people tolerate well:
- Start with posture reset: A few chin tucks
- Add neck motion: Gentle turns and side bends
- Open the chest: Doorway stretch
- Finish with shoulder blade control: Light squeezes or rows if instructed by your therapist
If you want more guided ideas, these easy exercises you can do at home to improve your posture fit well with cervical DDD self-care.
How to know if an exercise is helping
Good signs include less stiffness after movement, better posture awareness, easier head turning, or less tension during desk work. Temporary mild soreness can happen when you begin moving more. A major symptom spike that lasts is a sign to modify.
Use this quick check:
| Response | What it usually means |
|---|---|
| Feels easier after a few reps | Likely a good match |
| Mild stretch only | Usually acceptable |
| Sharp arm pain or increased tingling | Stop and reassess |
| Pain remains much worse later | Too much intensity or the wrong exercise |
Key takeaway: The best neck exercise is one you can perform well, consistently, and without feeding the pain cycle.
When Surgery Becomes a Necessary Conversation
The majority of individuals with cervical DDD do not need surgery. That is important to say clearly. Many cases improve with conservative care, better mechanics, and time.
Still, there are situations where surgery becomes an appropriate discussion. This usually happens when a structural problem is causing ongoing nerve or spinal cord compression, or when symptoms are progressing despite appropriate non-surgical treatment.
Signs that need prompt medical attention
A surgical conversation becomes more important when symptoms move beyond pain and stiffness alone.
Watch for concerns like these:
- Progressive weakness: The arm or hand is clearly getting weaker over time.
- Loss of coordination: Buttons, writing, or fine hand tasks become unusually difficult.
- Balance changes: Walking becomes less steady without a clear explanation.
- Persistent numbness that worsens: Especially if it follows a clear nerve pattern and keeps progressing.
- Pain that remains severe despite appropriate conservative care: Especially when daily function keeps declining.
These signs do not automatically mean you need surgery, but they do justify timely specialist evaluation.
What surgery is trying to do
When surgery is recommended, the goal is usually specific. It is not merely “fix neck pain.” It is more often to relieve pressure on a nerve or the spinal cord, stabilize a painful segment, or address a problem that has not responded to appropriate conservative treatment.
In plain language, a procedure such as an anterior cervical discectomy and fusion removes a problematic disc and creates more space where needed. That may sound intimidating, but in the right case, it is a targeted structural solution.
A balanced way to think about it
Fear pushes some people toward surgery too quickly. Fear keeps others away from necessary evaluation. Neither extreme is helpful.
A practical mindset looks like this:
- Start with conservative care when symptoms and exam findings support it.
- Monitor strength, sensation, coordination, and function.
- Escalate evaluation if neurological signs progress.
- Treat surgery as one tool for specific problems, not the default path.
That approach protects both your safety and your options.
How MedAmerica Rehab Can Guide Your Recovery
Living with degenerative disc disease in the neck is rarely about one perfect treatment. It is about learning what is driving your symptoms, improving how your neck handles daily life, and building a plan you can realistically follow.
That plan often includes guided exercise, hands-on care, posture retraining, ergonomic changes, and support during flare-ups. For many people, the biggest shift happens when they stop waiting for the neck to “settle down on its own” and start actively managing it.
In Deerfield Beach, MedAmerica Rehab Center brings together physical therapy, chiropractic care, acupuncture, and advanced shockwave therapy in one patient-centered setting. The clinic has served the community since 1995 and focuses on individualized, non-surgical care designed to reduce pain, restore movement, and help patients return to normal life with more confidence.
Whether your symptoms come from years of desk work, heavy lifting, a recent auto accident, or the slow buildup of tech neck, the right support can make daily movement feel less complicated. Clear guidance matters. So does a team that listens, explains, and adjusts treatment to your goals.
If neck pain, stiffness, arm symptoms, or posture-related flare-ups are limiting your day, MedAmerica Rehab Center can help you build a personalized recovery plan. Their Deerfield Beach team offers compassionate, evidence-based care for cervical spine pain and related conditions, with same-day appointments and a practical focus on helping you move better, feel better, and avoid unnecessary surgery whenever possible.

