How Long Does Workers Comp Take? A Florida Timeline
You lift a box, twist the wrong way, and feel that sharp pull in your low back. Or maybe your shoulder lights up halfway through a shift. At first, a common thought is, “Can I finish the day?” Then the bigger questions hit. “Do I tell my supervisor now? Who pays for treatment? How long does workers comp take? When do I get back to normal?”
That mix of pain, stress, and uncertainty is common. You're not only dealing with an injury. You're also dealing with forms, phone calls, lost work time, and the fear that a slow claim could slow your recovery too.
As a rehab provider, we see this confusion all the time. A patient comes in with sciatica, a shoulder strain, knee pain, or neck stiffness after a work injury, and the medical problem is only half the story. The other half is timing. If the claim moves slowly, care can start slowly. If treatment approvals drag, progress can stall. If paperwork is weak, you may spend energy defending your injury instead of healing it.
The good news is that workers' comp isn't random. It follows a process. Once you understand that process, the whole situation feels less overwhelming and much more manageable.
Your Work Injury Just Happened What Now
You report the injury, but your mind is still racing. Your back hurts when you stand up. Your boss says HR will call. Someone mentions insurance. Someone else hands you a form. You're wondering whether you should go to urgent care, whether you'll get paid if you miss work, and whether saying the wrong thing could hurt your claim.
That first day matters more than generally understood.
Workers' comp starts with notice. In plain language, that means your employer needs to know you were hurt and that the injury happened at work. If that step is delayed, everything behind it can slide too. Medical visits can get pushed back. Authorizations can take longer. Wage benefits may not start when you expect.
Focus on two things first
Your priorities are simple:
- Protect your health: Get evaluated and follow the treatment instructions you're given.
- Protect the paper trail: Report the injury promptly and clearly.
If you want a plain-English overview of what this type of coverage is designed to do, this guide to Workers Compensation can help you understand the basics before you get buried in claim language.
Practical rule: The faster you report the injury and get medical documentation started, the easier it is to connect your treatment timeline to your claim timeline.
A lot of patients also feel anxious about the first rehab visit. That's normal. If you want a simple preview of the intake process, paperwork, and evaluation flow, this page on what to expect can make that first appointment feel a lot less uncertain.
What people often get wrong
The biggest misunderstanding is thinking, “I'll wait and see if it gets better.”
That delay can create two problems at once. First, your pain may get worse. Second, the insurance side may start asking why you waited, whether the injury was really work-related, or whether something else caused it.
Early action doesn't guarantee a perfect claim. But it does put you in a stronger position medically and administratively, which is exactly where you want to be when you're trying to heal and get back to work safely.
The Workers Comp Journey A Step-by-Step Overview
Think of a workers' comp case like a road trip with checkpoints. Some trips are short and smooth. Others hit traffic, detours, and inspections. The overall route is usually the same.
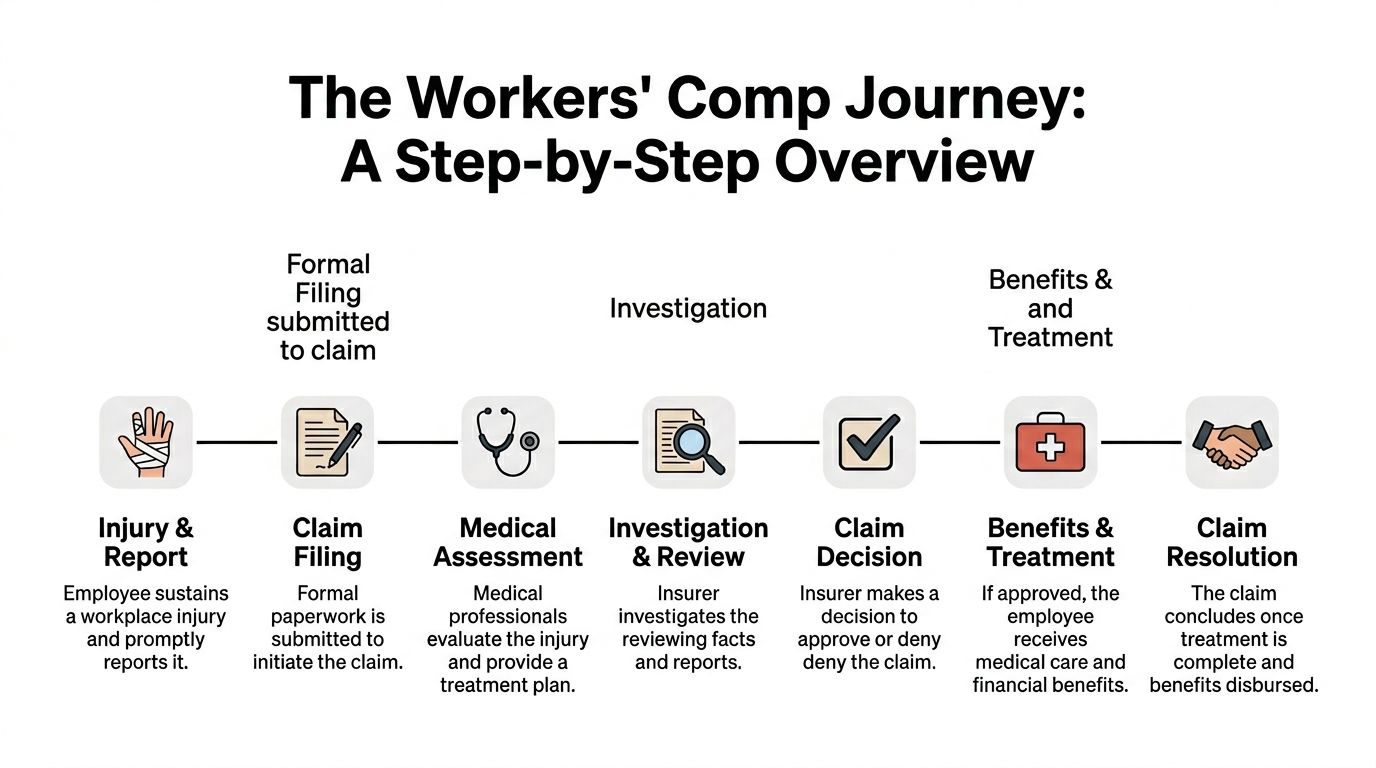
The seven checkpoints
Injury and report
You get hurt, then tell your employer. This is the moment the claim clock starts in a practical sense.Claim filing
The formal paperwork goes in. Your employer and insurer need enough information to open the file and begin review.Medical assessment
A doctor or rehab provider evaluates the injury, documents symptoms, and outlines a treatment plan. This step matters because the claim depends heavily on medical records.Investigation and review
The insurer looks at what happened. They may review records, compare dates, ask questions, or request more information.Claim decision
The insurer accepts the claim, denies it, or temporarily accepts it while continuing to investigate.Benefits and treatment
If approved, medical care and wage-related benefits can move forward under the rules of your state.Claim resolution
The case closes when treatment is completed, work status is clarified, benefits are paid, or the parties settle the claim.
How long each kind of case may take
Not every claim has the same timeline. According to benchmark data cited by Goldberg & Loren's California claim processing overview, simple claims resolve in 2-4 weeks, moderate cases such as back strains requiring physical therapy can take 6-12 months, and severe injuries can take 12-24 months. The same source says the National Council on Compensation Insurance reports an average resolution time of 16 months.
That range confuses people at first. They hear “workers' comp” and assume there's one standard answer. There isn't. A minor strain with prompt reporting and clean documentation may move much faster than a case involving surgery, disputed causation, or repeated treatment requests.
Why the stages connect to recovery
Each checkpoint affects the next one.
If reporting is delayed, filing may be delayed.
If filing is incomplete, investigation takes longer.
If investigation takes longer, treatment approvals may slow down.
If treatment slows down, your physical recovery can lose momentum.
Workers' comp isn't only a legal timeline. For many injured workers, it's also the calendar that controls when rehab starts, how consistently care continues, and how soon function returns.
A patient with a straightforward lumbar strain may begin treatment quickly and build progress week by week. A patient with the same diagnosis but a disputed claim may spend weeks waiting for authorization, then arrive deconditioned, stiff, and frustrated. Same body region. Very different recovery path.
A practical way to think about it
Use two timelines, not one:
| Timeline | What it covers | Why it matters |
|---|---|---|
| Claim timeline | Reporting, filing, insurer review, decision, benefits | Determines whether treatment and wage support move smoothly |
| Recovery timeline | Pain relief, mobility, strength, work tolerance, return to activity | Determines how long it takes your body to heal and function again |
When people ask how long does workers comp take, they're often asking both questions at once. They want to know when the paperwork will settle down, and when they'll feel like themselves again.
Why Some Claims Take Longer Key Factors That Cause Delays
A claim rarely slows down for just one reason. More often, delays happen when several small issues pile up. A missed detail in the injury report leads to extra insurer questions. Those questions delay authorization. Then treatment starts late, and recovery becomes harder to document clearly.

Delays caused by your side of the process
Sometimes the problem starts before the insurer even reviews the file.
- Late reporting: If you wait to tell your employer, the insurer may question when the injury occurred.
- Incomplete forms: Missing details force follow-up requests.
- Vague descriptions: “My back hurts” is less useful than a clear explanation of what happened, what body part was affected, and what symptoms began right away.
These aren't small paperwork issues. In rehab, details matter. If the original report says shoulder discomfort but your medical records later describe neck pain, arm numbness, and weakness, the insurer may stop and ask whether they're all part of the same injury.
Delays caused by the insurer
Insurers investigate because they want to confirm what happened and what care is medically necessary. That review can be reasonable, but it can also slow down the care you need.
For rehab-dependent injuries, the slowdown can be especially frustrating. According to the verified data summarized from this YouTube source, rehabilitation-dependent claims for injuries like sciatica or shoulder issues are 25% more likely to face temporary acceptance with a 90-day review hold, and insurer investigations can delay therapy authorizations by 1-3 months or more.
That matters in the clinic. A person with sciatica doesn't just feel “delayed.” They may sit less, walk differently, stop exercising, lose sleep, and become more fearful of movement while waiting for care to be approved.
A delayed authorization isn't only an administrative inconvenience. It can change the way an injury behaves in the body.
Delays caused by the injury itself
Some injuries are more complicated to manage.
When the medical picture is harder to pin down
A fracture seen clearly on imaging may be easier to document than pain that radiates, comes and goes, or overlaps with an older condition. Soft tissue injuries, repetitive strain problems, and cases involving multiple body regions often need stronger documentation over time.
That doesn't mean the injury isn't real. It means the medical record has to do more work.
Recovery can change the timeline
A claim may also lengthen because treatment itself reveals new information. A patient may start with low back pain, then show persistent leg symptoms, weakness, or difficulty tolerating work tasks. At that point, the care plan may expand, and the insurer may review the case more closely.
Three common patterns we see
| Delay pattern | What it looks like | How it affects recovery |
|---|---|---|
| Reporting gap | Injury wasn't reported promptly or clearly | Care starts later, symptoms may worsen before treatment begins |
| Documentation gap | Records don't fully explain function, pain pattern, or work limits | The insurer may question medical necessity |
| Authorization gap | Treatment requests sit in review | Rehab loses consistency, and progress may stall |
When you understand these delay patterns, the process feels less mysterious. You're not just waiting on “workers' comp.” You're watching specific moving parts that either support recovery or interfere with it.
The Florida Workers Comp Timeline Explained
Florida workers' comp feels confusing because the legal steps and the rehab steps overlap. You may be told your case is open, but a specific treatment request is still under review. You may be getting medical care, but not yet receiving wage benefits. Those are separate parts of the same system.
One Florida-specific point that catches many people off guard is the 7-day waiting period before wage benefits accrue, noted in the verified data drawn from the California-processing comparison source above. If you're out of work right away, that gap can create real stress while you're also trying to manage pain and appointments.
Florida deadlines and practical realities
Here is a simple reference point for the timing issues many people ask about.
Florida Workers' Comp Deadlines at a Glance
| Action | Deadline | Who is Responsible |
|---|---|---|
| Report the injury to the employer | As soon as possible under Florida practice | Injured worker |
| Wage benefit waiting period | 7 days before benefits accrue | Florida workers' comp system |
| Treatment approval review for rehab services | Can take weeks or months in utilization review | Insurer and utilization review process |
| Interstate claims processing | Can take 40% longer, or 45-60 days vs. 30, on average in the verified 2025 NCCI projection | Insurer and multi-state claim process |
The biggest Florida issue for many rehab patients is utilization review. According to the verified data cited by Pearson Koutcher Law, the utilization review process in Florida can delay rehab approvals by weeks or months. The same verified data says interstate claims in Florida's large tourism sector can take 40% longer, averaging 45-60 days versus 30, based on 2025 NCCI data presented in that source.
That projected interstate delay matters if your employer operates in more than one state, if payroll and insurance records are handled elsewhere, or if more than one carrier is involved. The medical need may be clear, but the file still has to move through a more complicated administrative chain.
Why this matters to your body, not just your case
A delay in physical therapy approval can mean you're waiting while your shoulder stiffens, your gait changes, or your back spasm pattern becomes more protective. In early recovery, consistency matters. Patients usually do better when treatment starts promptly, home exercises are reinforced early, and work restrictions are clarified before the injury becomes more stubborn.
Florida questions people ask most
- Who chooses the doctor? In workers' comp cases, treatment often follows the insurer's authorized provider process.
- Why is care approved in pieces? Because each service or phase of treatment may be reviewed for medical necessity.
- Why does one coworker's case move faster than another's? Because claim complexity, employer structure, and insurer review all vary.
If your claim is moving slowly in Florida, don't assume the injury is the problem. Sometimes the main delay sits in the authorization process, not the treatment plan.
If you want a legal overview that translates Florida claims into plain terms, this a detailed guide to workers' compensation claims in Florida is a useful companion read.
How to Shorten Your Workers Comp Timeline Practical Steps
You can't control every part of a claim. You can control the parts that most often create avoidable delays.

Report the injury right away
Don't wait for the pain to “prove itself.”
In strict systems, timing has real consequences. Verified data from Cardamone Law's Pennsylvania workers' compensation discussion notes that claims in Pennsylvania must be accepted or denied within 21 days of notice, and failure can lead to penalties of up to 50%. That same verified data underscores a practical lesson that applies broadly: late reporting by the worker is a primary reason for denial and delay.
Florida has its own rules and workflow, but the takeaway is universal. Prompt notice protects your care.
Be precise when you describe the injury
A strong report sounds like this: what task you were doing, when symptoms started, what body part was affected, and whether the pain changed your ability to keep working.
A weak report creates gaps. Gaps invite investigation.
Try to include:
- Body region: low back, right shoulder, neck, knee
- Mechanism: lifting, slipping, repetitive reaching, pushing, twisting
- Immediate symptoms: pain, numbness, tingling, weakness, stiffness
- Functional change: couldn't bend, couldn't finish shift, trouble walking, couldn't raise arm
Keep your records in one place
Save every document you receive. Write down dates of phone calls, clinic visits, work status notes, and approval requests.
That running timeline helps in two ways. It keeps you organized, and it helps you spot delays early enough to follow up before they become long gaps.
Follow the treatment plan consistently
When patients miss visits without explanation, stop home exercises, or fail to communicate setbacks, the record becomes less clear. The insurer may read that as lack of need, even when the underlying problem is pain, confusion, or scheduling trouble.
Keep this simple: show up, speak up, and make sure your records reflect what your body is doing day to day.
A timely first evaluation can help establish that medical record early. If you're trying to get care started, you can schedule an appointment so the injury, symptoms, and functional limits are documented clearly from the start.
Use your appointments well
Come prepared to explain what changed since the last visit.
Mention:
- Work tolerance: sitting, lifting, standing, carrying, overhead use
- Daily function: sleep, stairs, dressing, driving
- Symptom pattern: better, worse, radiating, more constant, triggered by specific tasks
Those details make your chart more useful. A useful chart supports treatment requests.
A short visual overview can help you think about the process in practical terms before your next step:
Follow up without disappearing
You don't need to call every hour. But you also shouldn't go silent for weeks if treatment hasn't been approved or your work note hasn't been updated.
A steady follow-up rhythm helps. Check claim status. Confirm that records were sent. Ask whether any additional forms are needed. Calm persistence often moves a file faster than frustration alone.
MedAmerica Rehabs Role in Your Recovery and Claim
Your treatment record does more than track pain. It helps explain why care is needed, what progress looks like, and what still limits your return to work.
That matters because workers' comp cases often rise or fall on documentation quality. If the notes are vague, the insurer may question ongoing therapy. If the notes clearly describe functional deficits, treatment response, and work limitations, the case is easier to understand.
What strong rehab documentation does
A good rehab team doesn't just record that you're in pain. They document how the injury affects movement, strength, tolerance, and job tasks.
That can include:
- Functional findings: trouble bending, lifting, gripping, walking, or reaching
- Treatment response: what improves after therapy and what still triggers symptoms
- Work capacity observations: whether you can tolerate modified duty or need restrictions
- Plan of care support: why additional visits or services remain medically necessary
Why that helps the claim move
Insurers review records to decide whether treatment is justified. Clear reports reduce guesswork. They also help everyone involved speak the same language, including the physician, adjuster, employer, and patient.
When records are timely and specific, treatment requests are easier to support. When progress is documented consistently, it becomes clearer whether you're improving, plateauing, or needing a change in strategy.
The best workers' comp rehab isn't just clinically sound. It's also well documented, because recovery has to be visible on paper as well as in the body.
If you need care for a work injury, this overview of workers' compensation rehabilitation explains how treatment, reporting, and recovery support fit together in one place.
The primary goal
The primary goal isn't to stretch out a case. It's to help you recover as efficiently as possible, with records that match what you're experiencing and a care plan that supports a safe return to work and daily life.
That's why the medical timeline and the claim timeline should never be treated as separate stories. They affect each other every step of the way.
Frequently Asked Questions About Workers Comp Timelines
Some questions don't come up until you're already in the middle of the process. These are usually the ones people ask after a delay, a denial, or a disagreement about treatment.
FAQ
| What if my claim is denied? | A denial doesn't always end the case. It usually means the insurer disputes some part of it, such as how the injury happened, whether it's work-related, or whether treatment is necessary. Your next step is to review the denial reason carefully and gather the medical and workplace documentation that addresses that issue. |
| Can treatment still be delayed even if the claim is open? | Yes. A claim can be active while a specific service remains under review. That's one reason patients get confused. They assume an open claim means all care is automatically approved, but treatment often moves through separate authorization steps. |
| Why does my case feel longer than someone else's? | Workers' comp timelines vary based on reporting quality, documentation, insurer review, and the nature of the injury. A straightforward strain and a more disputed rehab case won't move at the same speed. |
| Can I change doctors in a workers' comp case? | That depends on the state's workers' comp rules and the authorized provider process. In many cases, you can't freely switch the way you might with regular health insurance, so it's important to ask early how provider authorization works in your claim. |
| When do workers' comp cases end in settlement? | Some do, some don't. Settlement discussions often come later in a case when the medical picture is clearer, work status is better defined, and future care needs can be evaluated. |
| How long does workers comp take if I need rehab? | It often takes longer than anticipated because rehab care may require ongoing documentation and repeated authorization. The key is keeping treatment records consistent and responding quickly to any requests for information. |
If you're dealing with pain, paperwork, and a work injury claim at the same time, you don't have to sort it out alone. MedAmerica Rehab Center helps patients in Deerfield Beach move from confusion to a clear treatment plan, with experienced physical therapy and rehab care designed to support both recovery and the documentation your claim may require.

